
2 bodies believed to be from B.C. wash ashore Sable Island, N.S.
Nova Scotia RCMP say a boat containing the bodies of two people believed to be from British Columbia washed ashore the Sable Island National Park Reserve earlier this week.
There came a point during the pandemic, about nine months ago, when the staff at a pediatric clinic in Toronto was turning away at least 100 callers per day who were looking for a primary care provider.
At the same time, Kindercare Pediatric’s rostered patients were waiting longer than they should to see their own doctors. The way Kindercare owner Dr. Dan Flanders describes it, the scene was one of desperation.
"It became very, I don't know, distressing for everyone. Like, here we are, we have doctors and there's just an incredible need that's not getting met," he told CTVNews.ca in a phone interview on Jan. 27.
"It's hundreds of families a day saying, 'Our new baby needs a doctor, do you have any doctors for us?' And we would have to say, 'No, sorry, we don't.'"
That's about the time Flanders decided to hire two nurse practitioners and start an offshoot service called Kindercare365. The service launched on Jan. 26, after months of planning, allowing families who subscribe to access same-day virtual appointments, or same- or next-day in-person appointments, with a dedicated nurse practitioner, seven days a week. The catch is, there's a fee.
Starting at $29 per month or $290 per year, subscriptions give families access to what Flanders considers a stopgap until they're able to register with a family physician, or for times when there are no other, faster options.
"We are charging a reasonable rate for patients to have access to health-care providers who have the skill set and the licence and the capacity to help," he said.
"Another way to think of it is as a bridge until they find someone. It fills a gap, or sort of stretches like a bridge. It's just an added level of access."
This is one of the many options primary health-care providers in Ontario have turned to in order to meet increased demand for access to doctors in the past year while also managing staffing shortages and long-standing cracks in the province's under-funded health-care system.
Some fee-based virtual and telemedicine services have operated in Ontario since before the pandemic. Virtual care app Maple was launched in 2015 and operates across the country, charging patients $69 per appointment to see a Canadian-licensed general practitioner on demand, or $30 per month, paid annually.
One of Maple's main competitors is Telus Health MyCare, a virtual health-care app that provides free doctor’s appointments to residents covered by provincial health insurance in British Columbia, Alberta, Saskatchewan and Ontario, and charges for access to counsellors and dietitians.
It also shares the telemedicine market with services like Felix Health, a prescription service that charges a fee for online visits with a prescriber, and Tia Health, which is covered by the Ontario Health Insurance Plan (OHIP).
In the early days of the pandemic, primary-care clinics across Ontario pivoted to offer virtual and telemedicine appointments to avoid having patients visit in-person. For a while, the province allowed doctors to charge OHIP a certain fee for online visits.
However, the arrangement was only temporary. Last November, the province struck a new deal with the Ontario Medical Association and on Dec. 1, virtual care coverage dropped by about half. Some primary care providers responded by charging patients a new fee for those virtual services.
One of those providers was was KixCare, a virtual pediatric service established in 2021. When Alana Kayfetz and Matthew Kantor first began to use the service for their two-year-old son, Henry, it was covered by OHIP. Henry is medically complex, having been born with a connective tissue disorder, and it's important for him to avoid unnecessary exposure to viruses. So the free virtual appointments offered by KixCare were perfect for the family.
"It's a platform that allows parents and caregivers like us to access, quite frankly physicians," Kayfetz told CTV News Ottawa. "For example, we thought Henry had pink eye recently and we were able to get to that conclusion using a KixCare doctor."
When KixCare launched a paid service, KixCare360, in November, doubts about the platform began to sink in for Kayfetz and Kantor. KixCare now charges users a monthly subscription fee of $29 for virtual access to registered nurses, nurse practitioners and pediatricians.
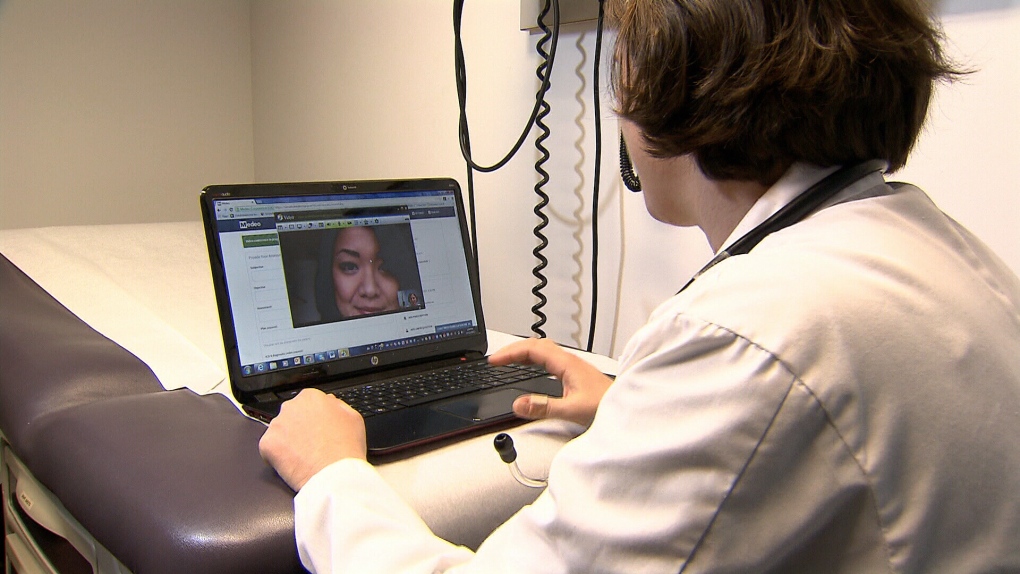 Virtual house calls that allow physicians to diagnose problems and prescribe drugs over the Internet are becoming increasingly popular across Canada. (File photo)
Virtual house calls that allow physicians to diagnose problems and prescribe drugs over the Internet are becoming increasingly popular across Canada. (File photo)
At a time when hospitals are overwhelmed and patients were waiting dozens of hours to see a doctor, Kayfetz said, the move felt wrong to her.
"Everything about this feels really weird and backwards," she said. "What we really don't want is for the ones who are the most fragile, our kids who are medically fragile…to not be able to see their primary care providers."
So if some primary care providers now charge for virtual appointments because they're no longer fully covered by OHIP, how can others, like Kindercare365, charge for in-person appointments?
It's uncommon for a primary care provider to charge patients for in-person access to a nurse practitioner – Kindercare owner Flanders said he couldn't think of any examples of another clinic doing what his is doing.
But according to health-care lawyer Christine Laviolette, it technically does not violate either the Canada Health Act or the Commitment to the future of Medicare Act in Ontario, both of which prohibit extra-billing patients for insured primary care services.
"Just because a clinic is offering virtual care services for a fee, does not mean that it is automatically in breach of the laws protecting our public health-care system," Laviolette, a health law group partner at Borden Ladner Gervais law firm, told CTVNews.ca in an email on Tuesday.
"One of the keys in determining whether a patient can legally be charged for a health-care service is determining who provides the service and the nature of the service."
Unlike family physicians, who bill their provincial governments for services rendered, nurse practitioners across Canada are paid by salary. In Ontario, nurse practitioners operating in hospitals or nurse practitioner-led clinics have their salaries paid by the Government of Ontario. Nurse practitioners working in a family physician's office, however, are considered independent contractors, so their pay is not covered by OHIP.
Because of this, and the fact that most of the extra-billing restrictions outlined by the federal and provincial health-care acts apply to physicians providing services that would otherwise be covered by provincial health insurance, Laviolette explained that "the same concern of a nurse practitioner receiving a payment from the province and a patient at the same time does not exist."
Questions of legality aside, Natalie Mehra believes charging patients for access to services normally covered by provincial health insurance, regardless of how they're delivered, violates the spirit of Canada's health-care laws.
"The reason why we have public medicare in Canada, is because people when they're sick, or their children are sick, when they're in need, they are not supposed to face a financial barrier to access care," Mehra, executive director of the Canadian Health Coalition, told CTVNews.ca in a phone interview on Monday.
"So this really throws that foundational principle of public medicare, and the ban on extra billing patients, into risk. Equity is the cornerstone to our public health-care system."
Mehra and the Ontario Health Coalition are among organizations calling on Premier Doug Ford to abandon plans to invest in private health care, and she blames the weakened state of the province's public health-care system for the proliferation of paid health-care services.
Ford announced in January his government plans to significantly increase the number of surgeries done in privately run for-profit clinics in order to reduce the backlog and shorten wait times for surgeries like knee replacements, hip replacements and cataract removal.
Mehra said the trend in Ontario toward shoring up public health care with private, for-profit health care is a sign the province's health-care system, ailing since long before the pandemic, is failing.
"I've done this for 27 years now. And, and I have never seen it so bad. You know, this is truly without exaggeration, the worst it’s ever been," she said.
"I mean, there have been problems in accessing doctors or in accessing care, but nothing like we're seeing today. I'm actually the most scared I have ever been."
Knowing what primary care providers in Ontario are dealing with, Dr. Allan Grill isn't surprised some have hired additional nurse practitioners to help spread the patient load.
Grill is a board member of the Association of Family Health Teams of Ontario and lead family physician of a family health team clinic in Markham, Ont. His team serves 26,000 patients and consists of 19 physicians, as well as nurse practitioners, dietitians and registered nurses.
He said the return of patients to in-person appointments as COVID-19 public health restrictions eased, the backlog of medical issues not treated during the height of the pandemic and the co-circulation of viruses like RSV, influenza and the common cold have all contributed to massive case loads for primary care providers this year.
"So when you combine the respiratory surge, and the fact that patients are more comfortable coming in, and the fact that a lot of care got delayed during the pandemic…we're extremely busy," Grill told CTVNews.ca during a phone interview on Tuesday.
On top of that, he said, large numbers of frontline workers across Ontario's health-care system have retired or left the field, citing burnout.
Grill said different clinics respond to these challenges in various ways, depending on their size, location and funding.
Unlike physician-owned primary care practices, which Grill said serve 75 per cent of Ontario’s patient population, family health teams are funded by the province. So if Grill decides to add a nurse practitioner to his staff, that person's salary is covered through public funding. For his team and their patients, that's a major benefit.
"Our nurse practitioners are amazing. They follow a bunch of patients, they help us with urgent care," he told CTVNews.ca. "The thing about having those members of your team is that if they can take some of the patients that have, you know… their condition is mild, that also opens up time for the family physician to deal with more complex cases that might be more within our scope."
Another way his team has pivoted to accommodate higher demand for primary and urgent care includes designating one physician to handle overflow when other physicians are overbooked with their own patients.
"Every day of the week, we actually have a doctor who is available to see patients from the other physicians' practices, in case that physician is not available," he said. "So for instance, they might be fully booked that day, or maybe they're away on vacation, or maybe they're off sick."
Grill said his team also all agreed to shift their schedules to accommodate a specific urgent care slot that is left open in their calendar each day for patients who don't have time to wait for an appointment.
"It's called same-day appointments, and they can only be booked that day," he said, "so that if somebody called in and they were sick, and they needed to be seen, it increased the chance they would see their own provider."
Grill said it's been relatively easy for his team to pivot, due to its size and funding. He imagines it would be harder for a smaller practice to reorganize itself the same way, or to add nurse practitioners whose salaries are not covered by OHIP.
"The family health team has set funding that the government gives to us that we can then go out and hire people. And then if over and above, we want to hire more as a physician group, we can definitely choose to do so," he said. "But boy, does it make it a lot easier when you have a lot of funding."
Ultimately, he wishes there were more funding for family health teams like his, and that no patient should have to pay for expedient care.
"We need to do more work to make sure that primary care is accessed equally for everyone in this province, no matter where you live, no matter who you are," he said.
"I feel very fortunate that when my patients come to see me, I'm able to offer them, these extra services at no cost to them. And I only wish that every patient in Ontario had the same access."
– With files from CTV News Ottawa's Tyler Fleming
The fee doctors can charge OHIP for virtual health care has been removed while awaiting clarification from the Ministry of Health.

Nova Scotia RCMP say a boat containing the bodies of two people believed to be from British Columbia washed ashore the Sable Island National Park Reserve earlier this week.
Pierre Poilievre says NATO allies treated Prime Minister Justin Trudeau like a human pinata at the leaders' summit this week — but he still won't commit to the alliance's spending goal.
Three men across Ontario are speaking out after losing hundreds of thousands of dollars to a cryptocurrency investment scam, including one man in Brampton who lost $226,000.
Joe Biden remains defiant that he'll remain in the U.S. presidential race despite a disastrous debate performance that triggered a wave of calls for him to end his candidacy.
With calls for Joe Biden to step down growing louder, many believe the U.S. president's press conference on Thursday was a 'make-or-break' moment.
A truck driver found a 1-year-old alive in a ditch off an interstate highway in Louisiana this week, a day after the boy’s 4-year-old brother was found dead near the same freeway in what investigators think was a case of abandonment around the time tropical storm conditions hit the area, authorities said.
A youth who disappeared during a flash flood in Wolfville, N.S., Thursday night has died.
One person has been hospitalized after falling from a swing ride at Canada's Wonderland.
Ben Affleck and Jennifer Lopez have added a tiny bit of fuel to the fire surrounding their marriage. Amid speculation that the pair are struggling in their relationship after marrying about two years ago, the couple has listed their 12-bedroom, 24-bathroom California home for sale.

A rare ammonite fossil – about 75 million years old - has been discovered in eastern Saskatchewan.
Seven-year-old goalie Hudson Hardill is an unlikely Calgary Flames fan, being that he lives in Peterborough, Ont., and his dad Chris is a Toronto Maple Leafs fan.
A WestJet employee's chance encounter on a recent flight spiced up her life in a big way.
A Kelowna, B.C., man says he's always liked gnomes because they have a 'bit of mystery' to them. And he recently got a taste of that whimsy when his garden gnomes disappeared, and came back to him in a peculiar fashion.
After more than 50 years, Toronto's iconic 'Leslieville dollhouse' will soon have a new owner.
One man is bringing a blast from the past to a Winnipeg community.
Some say a photograph is simply a memory frozen in time – and a high school graduation photo taken in Churchill, Man. takes that adage to a completely new level.
A rising track and field star overcame a big hurdle in his dream to represent Canada at the Olympics.
Would-be homebuyers who backed out of a deal to purchase a B.C. property in a hot real estate market have been ordered to pay the seller the difference between what they offered and what he was able to sell the home for when the market cooled.