TORONTO -- A disturbing trend is gaining ground in Ontario — more COVID-19 patients in the ICU who are younger and sicker than before, with the new variants blamed for these infections.
And some are so ill, their lungs so damaged, that they require a specialized form of care only available at a handful of hospitals to deliver oxygen to their bodies to keep them alive.
Dr. Niall Ferguson heads the ICU team at Toronto General Hospital — and he is clearly alarmed, calling the influx of cases “very concerning.
“Our ICU is already full today,” he said. “As are most of the ICU around the GTA. I think we're all quite concerned about what's going to happen in the next few weeks.”
The first two waves of the virus primarily hit people 50 and older. Now these ICU beds are filled with those decades younger, mostly infected with a variant of concern.
Claire Fielding, a clinical nurse specialist for critical care at the University Health Network, told CTV News that in the first wave, seeing a severely ill person who was in their 30s was a shock.
“Now it's this wall of people who are all in their 30s,” she said. “It's not a novelty anymore.”
She wants the public to know that, “Yes, this is a young person’s illness too.”
Most worrisome is that these younger patients are becoming very sick fast.
“Seems that variants of concern are now the dominant COVID-19 that's circulating in Ontario,” Ferguson said.
Because the variants are much more transmissible, “more patients and people who will get infected with variants are more likely to have severe disease,” he explained, “progressing much more quickly from being well [to] being extremely sick, over the course of just a few days.”
Their lungs are severely damaged, and so doctors say they need added life support.
That comes in the form of something called ECMO — which stands for extracorporeal membrane oxygenation.
“Essentially it's an artificial lung that we can use to support either just the lungs or the lungs and the heart together,” Ferguson said. “For COVID-19, [we] are mostly using it for lung support.”
When patients are hooked up to ECMO, blood is pumped into the machine, which takes out CO2 and puts in oxygen, before allowing the heart to pump that blood around to the rest of the body. The process takes the strain off the actual lungs, which have been damaged by COVID-19. It doesn’t replace a ventilator, but works alongside it.
“In this way, we treat the native lung more gently with a mechanical ventilator, we prevent further lung injury from happening, and give the lung time and opportunity to heal,” Ferguson said.
“We have 18 patients on here on ECMO [in] Toronto General today,” he added. "16 of them [because of] COVID-related critical illness. It’s our highest number so far.”
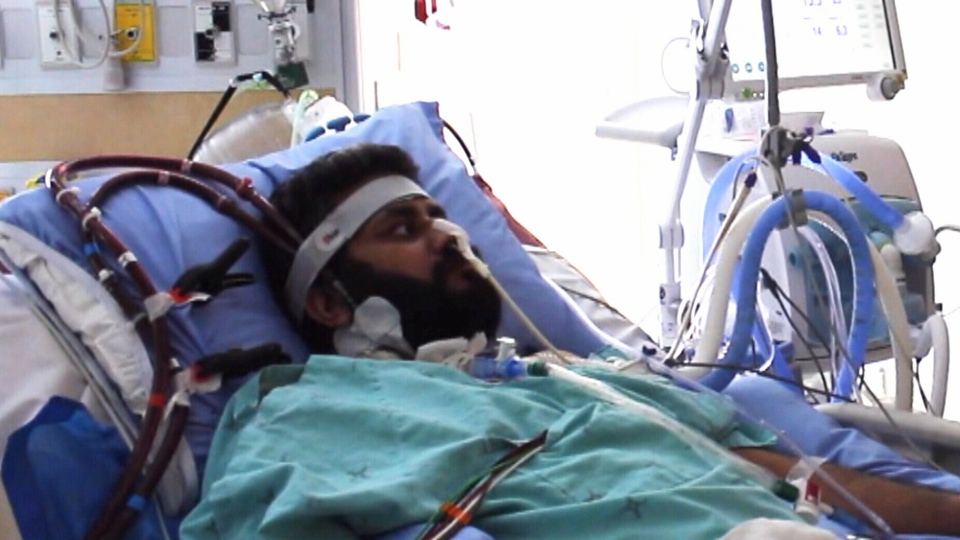
Jorawar Kandola is one of the patients at Toronto General. He has been on ECMO for seven weeks, and is showing signs of recovery.
His wife, Harreet, told CTV News that ECMO is “very helping.”
Ferguson said the 37-year-old had to be transferred to Toronto General to receive this specialized treatment because of how ill he was.
ECMO is for “when an ordinary mechanical ventilator isn't enough,” he said. “Obviously a very complicated and specialized intervention, so it's only done in specialized centers.”
Every day, Toronto General is being asked to take in three or four new patients needing this care.
“We're getting lots of calls about bringing patients who are in their 30s, 40s and 50s — even we've got a few [in] there, young 20s here with no past medical history,” Ferguson said.
But the hospital doesn’t have unlimited beds, and ECMO requires a lot of extra personnel to run.
“We have limited resources and spaces to put people,” Fielding said. “And so it's the fear of, how are we going to handle this?”
She said that people don’t seem to realize that every wave of the virus is growing.
“Wave three is hitting fast and furious,” she said. "It is really hard on us.”
“I'm really worried that things are getting out of control, just while we're nearing the finish line,” Ferguson added.
Most hospitals don't have the ability to offer the level of care that Toronto General can — only a handful have ECMO. So doctors are very concerned about what is going to happen in the next few weeks if cases continue exploding.
Over the span of just one week, between March 24 and March 31, the number of hospital beds occupied by COVID-19 patients across the country increased from 2,275 to 2,499 beds, with ICU patients increasing from 638 to 704.
And Ontario is suffering the worst, with 421 patients in the ICU as of Wednesday.
Ferguson said that he and his colleagues want to “show people that this really is real.
“People say hospitals are empty,” he said. “[But] they’re full of sick patients.
“Until everybody's well vaccinated, we all need to continue doing the same public health measures which we're getting tired of after a year, which are still very necessary.”