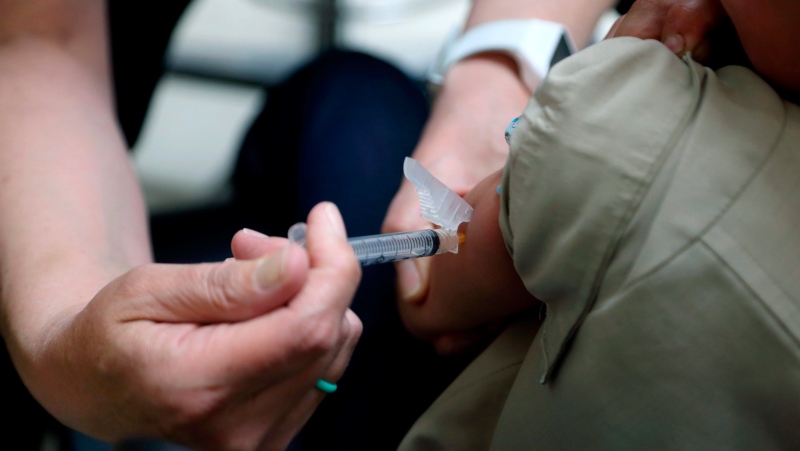
Not enough people are referred to allergists or prescribed EpiPens after experiencing mysterious allergic reactions, according to a new Canadian study.
Researchers at McGill University published their findings in The Journal of Allergy and Clinical Immunology: In Practice -- the first large-scale study of “anaphylaxis due to an unknown trigger,” or AUT, in Canada.
The research showed that one-fifth of AUT patients were not prescribed an epinephrine auto-injector such as an EpiPen, and only 56 per cent of AUT patients were referred to an allergist. The treatment and follow-up for patients with AUT was “suboptimal and inconsistent,” according to the research, which highlights the need for improved guidelines and educational programs across Canada.
“By increasing the knowledge regarding (AUT), we hope to improve the treatment of these cases and provide them better quality of life,” said lead researcher Dr. Moshe Ben-Shoshan, a pediatric allergist and immunologist at the Research Institute of the McGill University Health Centre. “It’s really challenging to treat these patients and it’s really important to refer them to specialists to make sure they get the right treatment.”
The new research is part of a larger project called Cross-Canada Anaphylaxis Registry (C-CARE), a database compiling data on anaphylaxis across the country.
While most anaphylaxis has identifiable triggers like food, medication, insect bites, latex and exercise, about 7.5 per cent of cases have unknown causes, according to the analysis of nearly 4,000 emergency room cases from 2011 to 2018. That makes it difficult for patients to avoid triggering substances.
Montreal’s Lia Davidson experienced anaphylaxis four years ago while playing sports, but doctors never determined why. Blood tests were even sent to Europe and the U.S., but nothing ever came back with a positive trigger ID. Unlike some patients with AUT, Davidson was prescribed an injector that she carries around with her.
“It is nerve-wracking knowing that it can happen at any time and I still don’t know what exactly caused it,” she told CTV Montreal.