Researchers say they have developed a simple and effective genetic-based test to detect certain gynecological cancers early on, in a breakthrough that offers new hope to the thousands of women who are diagnosed with the diseases each year.
Ovarian and endometrial cancers tend to be silent killers because they are difficult to detect before it might be too late. By the time the diseases are diagnosed, treatment options are often limited.
Because there isn’t any dedicated early-detection tests for ovarian cancer, diagnosis is usually dependent on the appearance of symptoms that are often vague and hard to recognize. In endometrial cancer, doctors also rely on signs such as abnormal vaginal bleeding to make a diagnosis.
That’s exactly what happened to Dominique Dagenais who was diagnosed with Stage 3 ovarian cancer in 2015. The 63-year-old woman told CTV News that she had few symptoms leading up to her diagnosis. She said she only had a bit of nausea and diarrhea before she found out about her cancer.
Dagenais underwent a total hysterectomy and several rounds of chemotherapy to treat her cancer.
It’s cases like Dagenais’ that inspired her doctor, Dr. Lucy Gilbert, to seek better screening methods for ovarian and endometrial cancers.
“It upsets me,” Dr. Gilbert said. “I am still doing exactly the same surgery and chemotherapy that we were doing when I started my career and I think it’s unacceptable.”
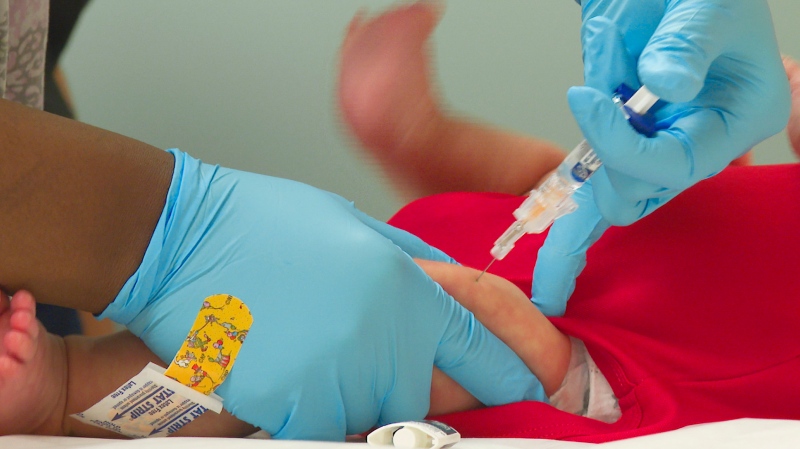
Dr. Gilbert, the director of Gynecologic Oncology at McGill University Health Centre in Montreal, worked with a team of researchers at her hospital and those in the U.S. and Europe to develop a modified Pap test called PapSEEK. Standard Pap tests are used to screen for cervical cancer.
For the first part of the study, the researchers used a regular Pap smear brush and analyzed the DNA in the sample to detect genetic mutations associated with certain gynecologic cancers. They tested it on 627 cancer patients and 714 healthy women.
By genetically analyzing the harvested cells, the new test was able to detect 81 per cent of the subjects’ uterine cancers and 33 per cent of the ovarian cancers.
Next, the researchers used a longer Tao brush to collect additional cells from the lining of the uterus. The minimally invasive tool allowed the study’s authors to harvest cells closer to the tumour sites.
With the longer brush, the detection rates went up and researchers were able to find 93 per cent of uterine cancers and 45 per cent of ovarian cancers. When the researchers also conducted a blood test as an additional screening measure for ovarian cancers, the detection rate went up to 63 per cent.
“This test goes to the very cause of the cancer,” Dr. Gilbert said. “It is the very earliest mutations that cause the cancer.”
Although the new test won’t help Dagenais, she said she hopes it will be able to prevent other women from going through what she experienced.
“Had I been earlier detected and went earlier myself, it would have been a big difference,” she said.
Dr. Gilbert said the researchers will need approximately four more years of study before it will be safe to use the new screening test.
“If we can find about half of these cancers early, it’s a huge breakthrough. That’s why we are so excited,” she said. “It’s the first time in my working career that I see hope.”
With a report from CTV News’ Avis Favaro and CTV Montreal’s Cindy Sherwin