There are “tremendous” differences in how cancer patients fare in high-risk surgeries across Canada, say the authors of a new report that found rates for complications and death vary widely from province to province.
The study commissioned by the Canadian Partnership Against Cancer found that death rates for some surgeries can be three to four times higher in some regions compared to others.
The solutions to the disparity, say the paper’s authors, is to create more “regional centres of excellence” – facilities where these high-risk, complicated surgeries are performed more often, and where they highly trained and experienced teams can perform them.
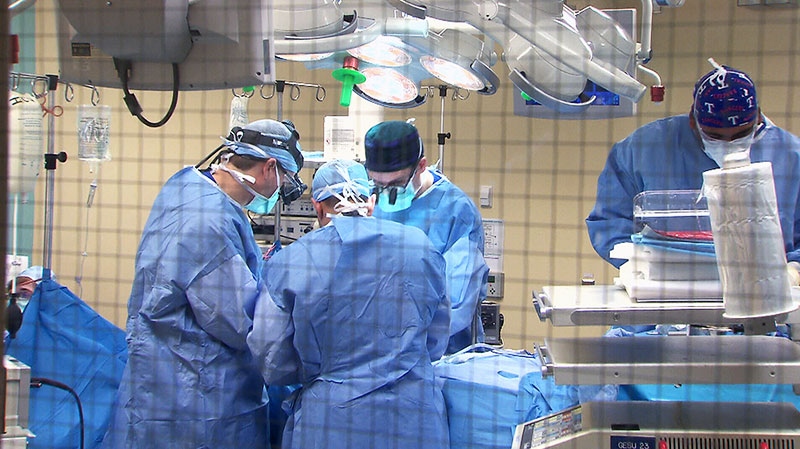
Dr. Christian Finley, a thoracic surgeon at St. Joseph’s Health Centre in Hamilton and lead author of the paper, says the study looked only at major surgeries for esophageal, pancreatic, liver, lung and ovarian cancers that typically result in long hospital stays and relatively high death rates.
“Even in the best hands in the world, they have an adverse event, or complication rate, of about 30 per cent. So these are large surgeries,” Finley explained to CTV News Channel Thursday.
“But on the flip side, these surgeries are probably the only way of getting cured of these cancers, so they’re very important to do. But they come with some degree of risk,” he said.
His team’s research found that the likelihood of receiving a potentially life-saving operation in a province where large numbers of that kind of surgery are performed can be double that of provinces with lower rates. As well, higher volume centres tend to have significantly lower risks of in-hospital mortality and shorter length of stays.
In the case of esophageal cancer surgery, for example, patients in Manitoba had an 11 per cent risk of dying in hospital over a nine-year study period, whereas the death rate during the same period in Newfoundland and Labrador was only 2.7 per cent.
Right now in Canada, though, there isn’t much regulation as to which procedures surgeons or hospitals should be allowed perform. Nor are there any rules about how frequently health professionals need to perform certain surgeries to ensure their skills remain up-to-date.
Finley says “regionalization” of high-risk surgeries to specific centres that specialize in them would benefit not only the patient, but health care teams as well.
Regionalization would provide more opportunities for surgeons to build their skills in complicated surgeries, and it would also encourage the development of specialized nurses, anesthesiologists, and radiologists.
These specialty centres would also benefit from having teams of experienced, well-trained physicians and surgeons who can confer amongst themselves to decide on best care.
Finley says the first step is to set standards and define what should be done where, as well as define what is needed in those facilities for those procedures.
All medical professionals want to improve survival rates for these types of complicated surgeries, Finley says, so the key is to set specific national standards, and collect more surgery data to help set benchmarks and improve surgical quality.
“By evaluating how we’re doing between provinces and between facilities and between surgeons allows us to look for the best of ourselves and to give focus to that,” he said.