Warning: Some readers may find some of the details in this story disturbing
Doctors in Australia are warning that a mysterious flesh-eating skin disease has become a "worsening epidemic" in one part of the country, and they are calling for help to learn how to stop it.
In a letter published Monday in the Medical Journal of Australia, a trio of doctors says incidents of Buruli ulcer have surged by 400 per cent in the last four years.
There were 275 new infections in the state of Victoria last year -- a new record and a 51 per cent increase over the year before.
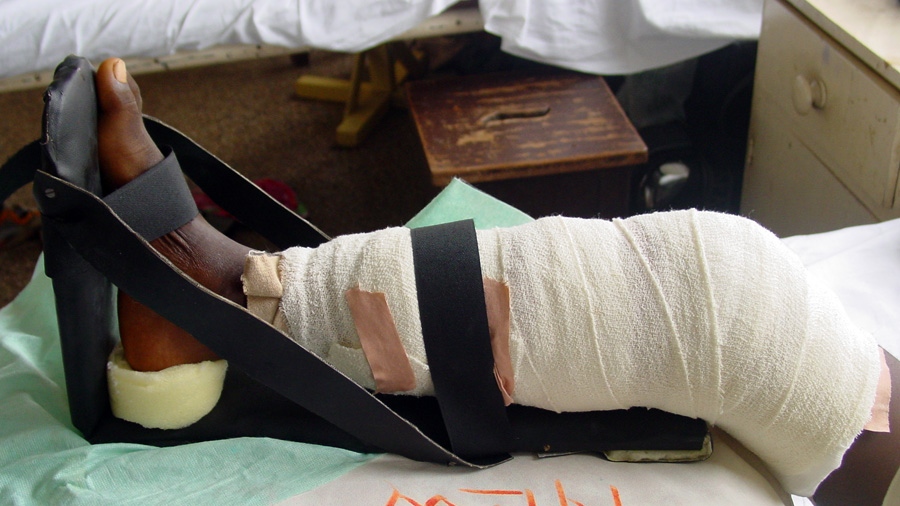
The disease “causes severe destructive lesions of skin and soft tissue,” the doctors write, causing painful large wounds, mostly on the arms and legs, that can spread all the way down into bone.
The disease can be treated with several weeks of antibiotics, though in severe cases, it can destroy muscle tissue and cause permanent disability or amputation.
But doctors don’t know how the disease is spread, nor how to prevent it.
Buruli ulcer itself is not a new disease. It has been reported in 33 countries in Africa, Asia, the Western Pacific, and South America, according to the World Health Organization.
Researchers also know the organism behind it: Mycobacterium ulcerans, which is from the same family of bacteria that causes leprosy and tuberculosis. But they don’t know how the bacterium enters humans.
The Australian doctors want help to understand why the number of infections is increasing and why infections are growing more severe.
They are also baffled as to why most of the Australian infections have been in the state of Victoria, while New South Wales, South Australia and Tasmania have been mostly spared.
The doctors write that although cases of Buruli ulcer has been diagnosed in Australia since 1948, efforts to control it have been hampered because its “mode of transmission” remains unknown.
“It is difficult to prevent a disease when it is not known how infection is acquired,” write the authors, led by Dr. Daniel O’Brien, an associate professor of infectious diseases at the University of Melbourne.
One theory is that the disease is spread by mosquitoes or aquatic insects. Another possibility is that it lives in the feces of animals such as possums that then enters waterways. A third theory is that it lives in contaminated water or soil and enters humans when they breathe in contaminated spray or dust, or it enters the skin through cuts and scrapes.
The doctors say what is needed now is urgent research.
“As a community, we are facing a rapidly worsening epidemic of a severe disease without knowing how to prevent it,” they write.
“…It is only when we are armed with this critical knowledge that we can hope to halt the devastating impact of this disease.”