In a few weeks, Lynda Millard will run out of a medication that has been critical to her digestive function since she had three feet of her small intestine removed in 2015.
Cholestyramine is used to treat high cholesterol and remove bile acids from the body. Most digestion and absorption of food takes place in the small intestine, and patients like Millard often suffer from a condition called bile acid diarrhea, which can severely impact quality of life and lead to dangerous vitamin and mineral imbalances. Cholestyramine helps manage this condition.
Unfortunately for Millard and patients like her, it's one of more than 1,800 drugs currently in shortage in Canada.
"I can no longer get this medication," 75-year-old Millard, told CTVNews.ca in an email. "Everywhere I have called I've been told it's back-ordered until 'some time in 2024.' My Doctor contacted a gastroenterologist and was told there is no substitute available as other brands have been discontinued."
Experts say the number—and length—of drug shortages has gradually increased in this country over the last decade or so, putting patients like Millard in difficult, and sometimes dangerous, positions. Potential solutions like rethinking where drug manufacturing is concentrated and expanding pharmacists' prescribing privileges could help ease the impacts on patients, they say.
In a follow-up interview with CTVNews.ca on Wednesday, Millard said her doctor advised that if she can't fill her prescription in Canada when her current supply of the drug runs out, she should travel to the United States to try and find some, or take "original Metamucil and then add some Imodium," and hope for the best.
"It's been extremely stressful the past couple of weeks while I searched for this stuff," she said. "I can't live without this stuff. I have to have it."
Health Canada's public data on drug shortages only goes back as far as 2017, because that's when legislation requiring manufacturers to report shortages took effect, but the agency told CTVNews.ca that in 2019, "shortages were beginning to last longer" than they had the previous two years.
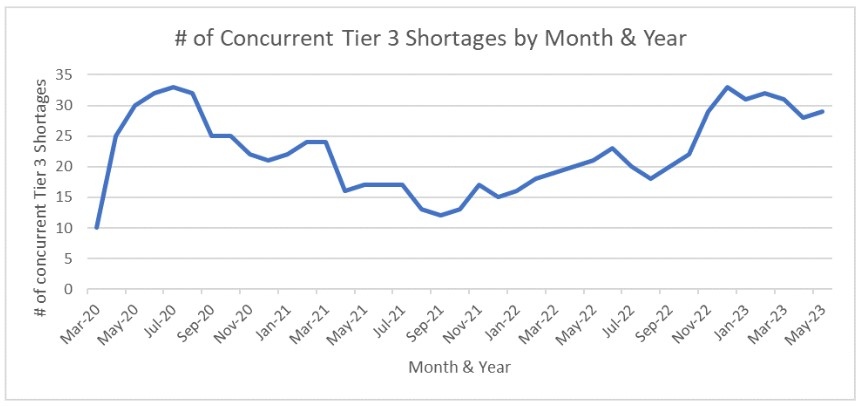
During the peak pandemic years of 2020 and 2021—the time of masking, physical distancing requirements and gathering limits—the number and duration of shortages dropped temporarily. However, Health Canada recorded an uptick in 2022 that marked a return to the pre-pandemic numbers, and that trend has continued throughout 2023.
Pharmacist Jen Belcher believes the problem started much earlier than 2019, however.
"Drug shortages overall over the last five to 10 years have been much greater in quantity and severity than we've ever seen before," Belcher, who is vice president of strategic initiatives for the Ontario Pharmacists Association, told CTVNews.ca in a phone interview.
"It's been challenging for pharmacies to manage."
One of the ways pharmacists manage shortages is by prescribing alternative drugs themselves, if they have sufficient prescribing privileges. Lacking those privileges, they work with the original prescriber to suggest alternatives.
Belcher said pharmacists in most provinces have the ability to prescribe alternatives themselves. In jurisdictions like Ontario, Manitoba and the Northwest Territories, she said, they don't. For pharmacists in those provinces, the back-and-forth with prescribers over alternative medications can be especially time-consuming.
"That does create additional challenge workloads for the pharmacies and the prescribers because those prescribers now need to receive that communication and action it and respond to us, and we need to be following up if necessary," she said.
In fact, surveys by the Canadian Association of Pharmacists have found pharmacy teams across the country spend, on average, 20 per cent of each day just managing shortages.
"There's a lot of work that's done at the pharmacy that most people wouldn't see, and there's a lot of attempts to source medications from multiple sellers. Sometimes, pharmacies will supply each other when there's a shortage situation," Dr. Barry Power, chief pharmacist at the Canadian Pharmacists Association told CTVNews.ca in a phone interview. "Some pharmacies will also compound alternative products, if it's possible."
Power said he hasn't noticed a dramatic increase in the number or duration of shortages in recent years, but said they've been a problem for decades.
"We're always experiencing shortages. And it goes back to prior to the pandemic," he said.
GLOBAL PROBLEMS, LOCAL IMPACTS
While shortages arise due to a number of fluid and situational reasons—such as manufacturing disruptions, increased demand, delays in shipping and raw ingredient shortages—he said some of the factors that make the industry so susceptible to a few of these also go back decades.
These include the consolidation of drug manufacturing companies, the globalization of manufacturing and the concentration of manufacturing into certain regions.
According to Robin Feldman, director of the University of California Hastings Center for Innovation, the number of leading pharmaceutical companies fell from 60 to 10 between 1995 and 2015.
"In 2017, just four companies produced more than 50 per cent of all generic drugs," Feldman told the U.S. House of Representatives during a hearing about consolidation in the health-care industry in 2021. Moreover, Power said manufacturing has increasingly been concentrated in countries overseas. A 2020 report by law firm Norton Rose Fulbright reveals that as much as 60 per cent of active pharmaceutical ingredients are produced in China, while 70 per cent of finished pharmaceuticals are produced in India.
"This translates to 70 per cent of all finished prescription drugs in Canada and 90 per cent of all components used in drugs manufactured domestically originating from abroad," the report reads.
Experts say all of this consolidation and concentration creates an "all your eggs in one basket" scenario that can easily destabilize Canada's drug supply.

"A lot of the drug manufacturing has been consolidated into, you know, China and India, and there's very little domestic production that happens anymore," Power said. "So anything that happens in these foreign drug supply regions will affect."
If one drug manufacturing plant or segment of a supply chain is brought down by a natural disaster, political instability, shipping delays or some other unforeseen issue, Power explained, entire countries could face drug shortages, with few alternatives for sourcing the products affected.
This is what happened in 2017 when Hurricane Maria swept through Puerto Rico, leaving mass death and destruction in its wake.
"Almost all of the sterile solutions for the United States were manufactured in Puerto Rico, so for quite a while there was a U.S.-wide shortage of intravenous solutions for hospital use," Power said.
On the other hand, while Puerto Rico is also the manufacturing hub supplying Tylenol brand acetaminophen "just about everywhere," Power said, most of Canada's Tylenol acetaminophen is manufactured in Guelph, Ont.
"So there is some domestic supply and that can shield us from international shortages," Power said. "So we never saw an impact from the hurricane."
PHARMACISTS CALL FOR MORE RESILIENCE
Drug shortages have become a stubborn facet of health-care in Canada over a period of many years. But that doesn't mean their impacts can't be lessened.
Power believes work already underway by the drug shortages unit at Health Canada to source imports from a wider range of manufacturers could help safeguard Canada's supply in the face of future shortages.
"(During) the pandemic, this group was given authority to work with manufacturers to import medications from other countries in cases where it was looking like we were going to be without any medication in Canada," he said. "There were some high profile situations where that power was enacted."
When Canada experienced a shortage of children's pain and fever medicine in late 2022, the federal government responded by importing the drugs from the United States. It did the same thing earlier in the pandemic amid a shortage of asthma inhalers, sourcing the inhalers from South America and the United Kingdom.

"So there has been some improvement in the way we can respond to shortages," Power said.
There is also room for improvement in the way health-care providers respond to shortages, according to Belcher.
Belcher said every province should grant pharmacists the ability to prescribe a wider range of medications, because it would allow them to more nimbly find workarounds when problems caused by shortages arise.
"All of our scope of practice is provincially regulated, and it looks different across the country," she said. "Alberta really is the most expansive in terms of scope of practice for things like prescribing. Their pharmacists can prescribe independently for any Schedule One drug, whereas here in Ontario, we're really limited."
Finally, Belcher hopes to see the federal government collaborate more with industry leaders, health-care providers, provincial and territorial leaders and other stakeholders to continue developing solutions to the issue of shortages.
"There need to be a lot of multi-stakeholder conversations to look at what we need to do as a nation to ensure Canadians continue to have access to the medications they need for their health conditions and we are a country that has a stable and resilient drug supply," she said.































