An Ontario man says he’s at his wit’s end after his wife spent five days in a hospital hallway, waiting for a psychiatric care bed.
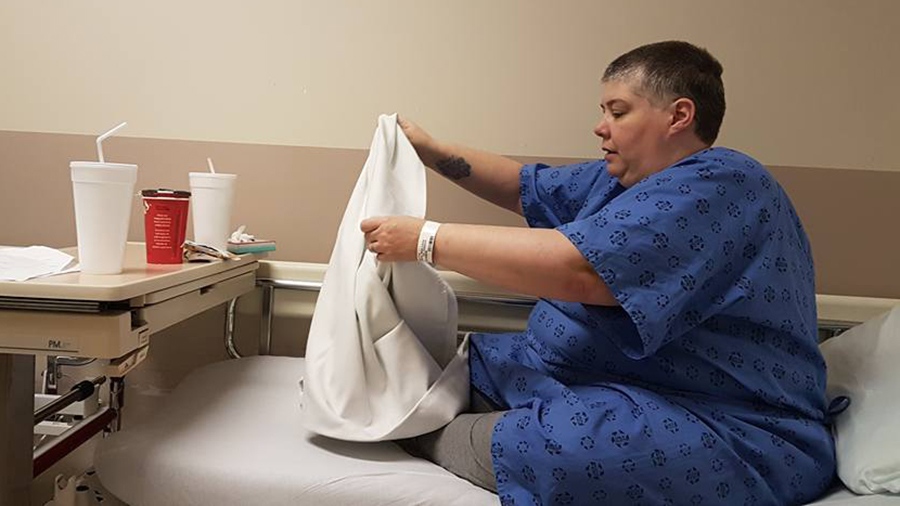
Dawn Warren, who suffers from chronic depression, was taken to Victoria Hospital in London, Ont., by ambulance last Thursday. Her husband, David Warren, said he found her unresponsive when he came home from work and called 911.
When his wife arrived at the hospital, she was assessed and placed on a gurney in a hallway because no beds were available, Warren said. She didn’t receive a proper bed in a hospital room until five days later, on Tuesday.
“It’s been very frustrating,” Warren told CTVNews.ca in a telephone interview this week. “What we need is more beds.”
In a brief phone conversation with CTVNews.ca from the hospital before she received a bed, Dawn Warren, 48, said there were several other patients in the hallway with her. She said she was able to speak to a psychiatrist while she waited for a bed.
Her husband said the local health-care system is ill-equipped to deal with patients who require mental health care, especially when it comes to emergencies. He also said that Dawn hasn’t had a regular psychiatrist for the past six months after her doctor resigned.
“She fell through the cracks,” Warren said.
He said that his wife has faced long wait times before, prompting him to meet with hospital officials in the past to suggest improvements to psychiatric care, but not much has changed.
In a statement to CTVNews.ca, the London Health Sciences Centre (LHSC), which includes Victoria Hospital, said it has been experiencing “longstanding significant pressures in our mental health care capacity,” like many other hospitals across Ontario.
“Our current volume and wait-time realities mean that we have admitted patients in unconventional surge spaces and I want to acknowledge the hardship this situation causes for the patients and families impacted and apologize for any inconvenience and stress that has resulted,” Julie Trpkovski, LHSC’s vice-president of mental health, emergency services and access and flow, said in the statement.
She said the region’s mental health-care system has struggled with increasing demand, “and we continue to work collectively to better meet patient and family needs.”
Peggy Sattler, the NDP MPP for London West, has discussed Dawn Warren’s plight with her husband in the past. She has been highlighting local health-care issues in the provincial legislature for years and says that stories like Dawn’s are not uncommon.
Sattler said “a frantic husband” came to her office last year after his wife had been lying for a week on a stretcher in a hospital hallway, waiting to be placed in the psychiatric care unit.
That patient, Angela Cameron-Jolly, shared her story with the local media. Her case was just one example of an overtaxed mental health-care system, struggling with a shortage of psychiatrists and resources, Sattler said.
As “mental health needs in the community seem to be increasing,” more than $140 million has been removed from LHSC’s budget in the years that Kathleen Wynne has been Ontario premier, Sattler told CTVNews.ca in a telephone interview.
She said a lack of co-ordination among mental health-care services in London means that many patients end up in the emergency room, where they spend days waiting for a bed only to later be discharged without proper community support. Without regular outpatient mental health care, those patients end up back in the ER, creating a vicious cycle, Sattler said.
“It’s been an ongoing crisis,” she said. “There’s this incredible pressure on emergency (rooms).”
In a statement to CTVNews.ca, Ontario Health Minister Helena Jaczek said that improving access to mental health care is “a priority for this government.”
She said the province provided LHSC with more than $1.7 million in base funding last fall to open an additional 24 mental health beds. That amount was increased and made permanent starting this year, for a total of $5.5 million in new annual funding going to LHSC “to improve access to care for those with acute mental health needs,” Jaczek said Wednesday.
She said the new funding will also go towards a new mental health unit and the hiring of five additional psychiatrists, nurses, social workers and occupational therapists.
The Ministry of Health acknowledged that “timelyaccess to hospital and community mental health programs have been challenging” amid growing demand for services. The Liberal government said that’s why it is making a “historic investment” of $2.1 billion over four years in mental health and addictions services across the province.
On Wednesday, David Warren said he is happy that his wife is finally getting the proper medical attention she needs, but he will continue to speak out about the lack of hospital beds and long wait times.