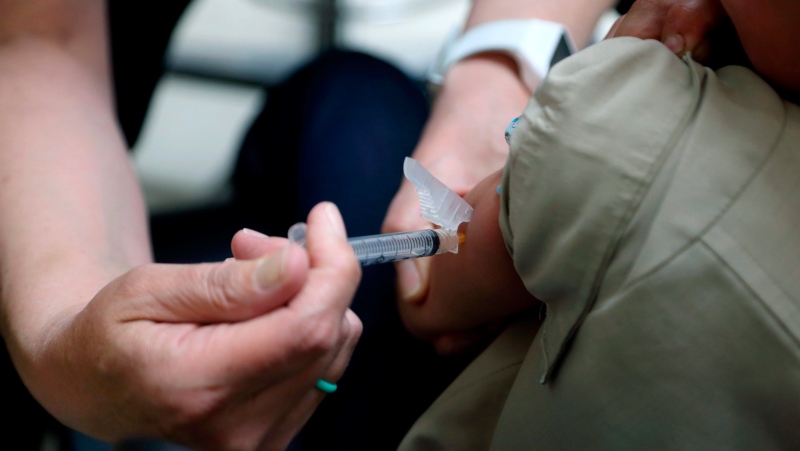
A study surveying American women showed that one third of women who take hormones at menopause are using compounded hormones. Of the reasons cited for choosing compounded over approved hormone therapy options is respondents thinking hormones are safer and offer more benefits than approved therapies.
Some 3,700 women age 40 to 84 took part in the survey that asked about their hormone use at menopause, what they thought the benefits would be, what benefits they got, what side effects and health problems they experienced, and more.
But one concern arising from the study is four reports of endometrial cancer among women who took compounded hormones.
Results
About 1,000 of the respondents had used or were using hormone therapy during menopause. Thirty-one per cent of hormone therapy users were taking or had taken compounded hormones, and 34 per cent were taking them at the time of the survey.
Some 42 per cent of the women who took compounded hormones thought that "natural" or "bioidentical" hormones are safer than other types of hormones, even though there are more than 30 tested and approved hormones for menopause, including many that are similar to human hormones.
It is important to note that marketing things under the name "bio-identical" and "natural" often equates to safety in the consumer's mind. However that is not the case. The authors note that the term "bio-identical" has no basis in science and should be dropped from medical jargon.
These are simply compounded hormones, period, and concerns with compounding include that the hormones are not regulated and often there is great variability in the final end product. For women with an intact uterus there must be adequate progestogen protection to protect the lining of the uterus when using any form of estrogen.
Although side effects of hormone therapy were not common among the survey respondents, the women who used compounded hormone therapy reported higher rates of vaginal bleeding and acne than women who used approved hormones.
As mentioned, four women who used compounded hormones reported they had endometrial cancer, cancer of the uterine lining, whereas none who used approved hormones reported a case.
Most women who used either compounded or approved hormones (about 70 per cent of each group) took them for hot flashes—the major, approved indication for menopausal hormone therapy.
But women who took compounded hormones more often expected unproven benefits that are not approved hormone therapy indications, such as the improvement of moodiness or irritability, sleep, low energy, depression, muscle mass, memory or concentration, sexual desire, and overall appearance as well the prevention of aging and an ability to lose weight.
Clinical trial, prescribing, and post marketing data are all available to tell us how safe and effective approved hormone therapies are, but none of that is available for compounded hormone therapy.
As the authors point out: "Because so many women are using these untested therapies with unknown risks, we need to find out what those risks are."
The suggestion is that mandated, centralized reporting of prescriptions filled by compounding pharmacies would be a better approach, and the benefits and risks can be determined only by randomized clinical trials.