The Supreme Court of Canada has dismissed an appeal by doctors at a Toronto hospital who sought to withdraw treatment from a severely brain-damaged patient they say has no hope of recovery.
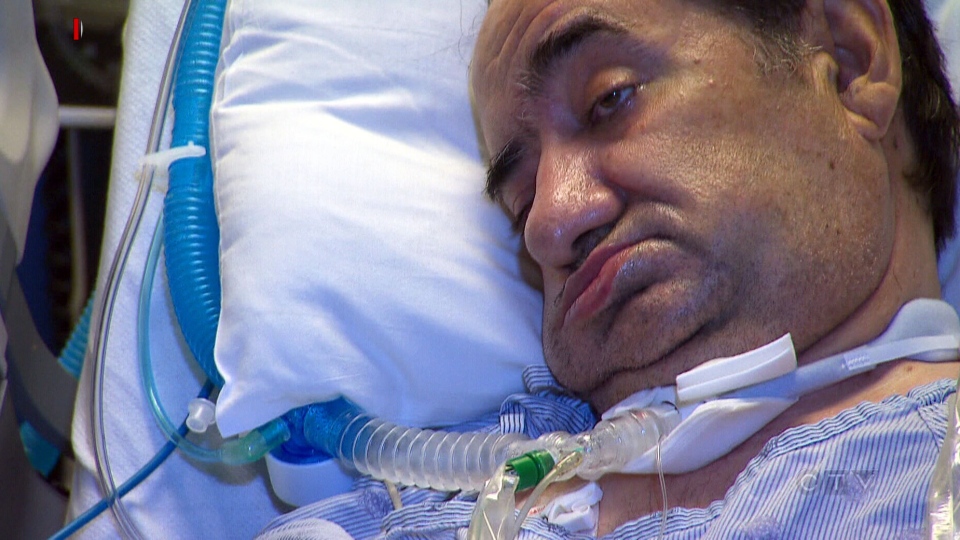
The case centres on Hassan Rasouli, 61, who has been on a ventilator at Toronto's Sunnybrook Health Sciences Centre since October 2010, when he developed meningitis and severe brain damage following surgery to remove a brain tumour.
His doctors believe keeping him on the ventilator is ineffective and no longer in his best interest and that he is likely to die from one of the many complications related to being permanently confined to a hospital bed.
But Rasouli's wife, Parichehr Salasel -- who is a family physician in her home country of Iran and Rasouli's designated substitute decision maker -- refused consent to withdraw life support.
She and her daughters argued that Rasouli is in a minimally conscious state, responds to stimulation and appears able to communicate with them.
Two lower Ontario courts sided with Rasouli's family on the matter. They ruled that under Ontario's Health Care Consent Act, Rasouli's doctors need to have Salasel's consent to withdraw life support, and that if she refused, they would need to refer the case to the province's Consent and Capacity Board.
But rather than go to the Board, Rasouli's physicians, Dr. Brian Cuthbertson and Dr. Gordon Rubenfeld, appealed directly to the Supreme Court.
In Friday's 5-2 decision, Chief Justice Beverley McLachlin writes that the Health Care Consent Act (HCCA) provides a mechanism for resolving the dispute. She also said that under the act, medical treatment is more than just what doctors consider to be of "medical benefit" to a patient and that even end-of-life care is a treatment.
"While the end of life context poses difficult ethical dilemmas for physicians, this does not alter the conclusion that withdrawal of life support constitutes treatment requiring consent under the HCCA," she wrote for the majority.
Rasouli's physicians argued consent was not required to withdraw life support where such treatment is futile. But the court disagreed.
"By removing medical services that are keeping a patient alive, withdrawal of life support impacts patient autonomy in the most fundamental way," McLachlin wrote. "The physicians’ attempt to exclude withdrawal of life support from the definition of 'treatment' … cannot succeed."
For Hassan Rasouli's doctors, the decision means must now refer the matter to the Consent and Capacity Board, since the family will not give consent to withdraw life support.
Case likely to return to Consent and Capacity Board
Criminal lawyer Edward Prutschi, of CrimLawCanada.com, says it appears the court did not want to hand doctors the right to make such decisions all on their own, contrary to the wishes of the family.
"And that's the reason that Ontario has a Consent and Capacity Board that is made up of doctors and ethicists, which will make the determination," Prutschi told CTV News Channel.
"And so the Supreme Court has said, 'Look, there's a system in place when this type of decision is contemplated. This meets the definition of treatment. Don't come to us; go to them'."
Mark Handelman, a lawyer and former member of the Consent and Capacity Board, says the board is comprised of doctors, psychiatrists, community members and lawyers such as himself. He maintains that the board is better equipped to resolve life support cases than the courts.
"It's probably heard more end-of-life care cases than all the courts in Canada put together," he told CTV News Channel. "It is an expert tribunal. They've heard these cases since the Health Care Consent Act was enacted in the mid-90s. And while it's not perfect, it's better than forcing people to start lawsuits and go to court on these matters."
Family hopeful for further recovery
Following the decision, Salasel told reporters she was pleased with the decision and reiterated that she believes that her husband is aware.
She said for the first three months after the meningitis, Rasouli was in a full coma, but she believes he has since improved and now "understands everything that happens around him but he cannot respond."
She told reporters she believes her husband wants help and she will do everything she can to help him.
Dr. Charles Weijer, a physician and bioethicist at University of Western Ontario, says the Supreme Court has upheld the notion that patients and families have a voice in end-of-life decisions.
"How we die is an enormously important part in everyone’s life; it’s the final act and the final chapter," he told CTV News.
"That doesn’t mean that patients and families can dictate precise treatment they're going to receive at end of life, but upholding notions like patient dignity, autonomy and values requires that we give voice to patients and families in these decisions."