Medical authorities are alarmed by an emerging fungus causing fatal infections that are difficult to diagnose and resistant to traditional drugs.
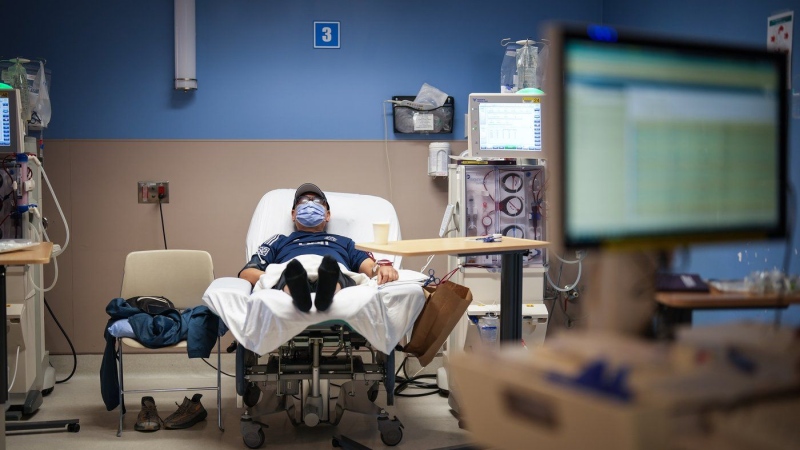
Candida auris is designated “a serious global health threat” by the U.S. Centers for Disease Control and Prevention. More than one in three patients with invasive C. auris infection dies. The fungus is easily picked up and spread between people and can survive for weeks on surfaces, including in hospitals where patients have been treated.
There have been only a handful of cases in Canada to date, but a rise in antifungal resistance comes amid long-standing and growing concern about the overuse of antibiotics that is lowering the effectiveness of anti-bacterial drugs. Anti-microbial resistance has been called a “global health emergency” by the United Nations, which says it could lead to more deaths annually by 2050 than the eight million caused by cancer.
The emergence of C. auris has been rapid. It was first isolated in an ear infection in a patient in Japan in 2009, and has since been found in about 30 countries.
The Public Health Agency of Canada says the first known case in Canada appeared in 2017, in a patient reporting two years of ear infections that required hospitalization following a trip to India.
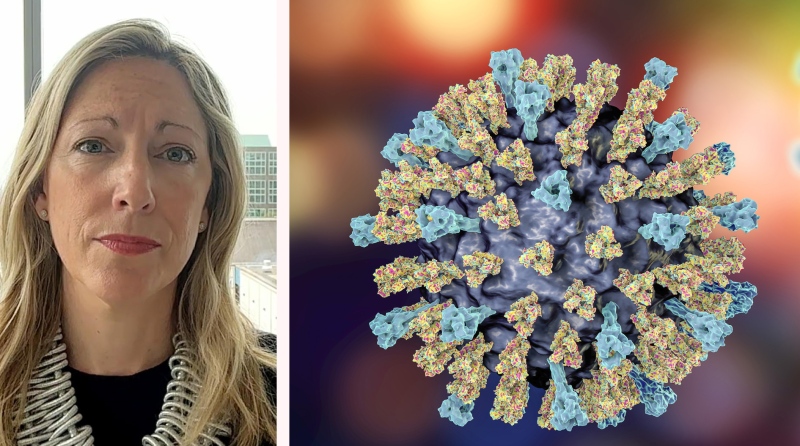
“Fortunately in Canada, we are well prepared for this and there is great lab capacity across Canada and we are well aware that this infection is out there,” said Dr. Isaac Bogoch, an infectious disease specialist at Toronto General Hospital.
This fungus is tricky to diagnose using traditional lab techniques and it’s resistant to many drugs that would normally be used to fight it. The key is suspecting this strain of fungus and immediately using drugs that are typically only prescribed after first-line choices don’t work, says Bogoch, who is an associate professor at the University of Toronto.
“Having said that, it is still quite concerning that this seemingly appeared out of nowhere and is starting to pop up in different countries in the world. Luckily, it is still a rare infection,” he told CTV’s Your Morning Friday.
Bogoch says the infection typically preys on those in hospital, who are hooked up to intravenous lines or taking antibiotics.
“It doesn’t seem to infect healthy people for the most part.”
Most C. auris cases in the United States have been detected in the New York City area, New Jersey, and the Chicago area, says the CDC.
Last May, an elderly man admitted to Mount Sinai Hospital in Brooklyn for abdominal surgery was found to have an infection caused by C. auris. He died after 90 days in the hospital, but the fungus was found everywhere in his room. The hospital needed special cleaning equipment and had to rip out some of the ceiling and floor tiles to get rid of it.
“Everything was positive — the walls, the bed, the doors, the curtains, the phones, the sink, the whiteboard, the poles, the pump,” Dr. Scott Lorin, the hospital’s president, told the New York Times. “The mattress, the bed rails, the canister holes, the window shades, the ceiling, everything in the room was positive.”
Bogoch says there is research underway to understand more about the fungus, including why it’s resistant, how it spreads and how it can be prevented from making people sick.
According to the CDC, there are millions of species of fungi on Earth, but only about 300 are known to make people sick. Fungal infections are often caused by microscopic fungi common in the environment. Fungi live outdoors in soil and on plants as well as on many indoor surfaces and on human skin.
Fungal infections range from skin infections such as ringworm to lung infections to fungal meningitis.