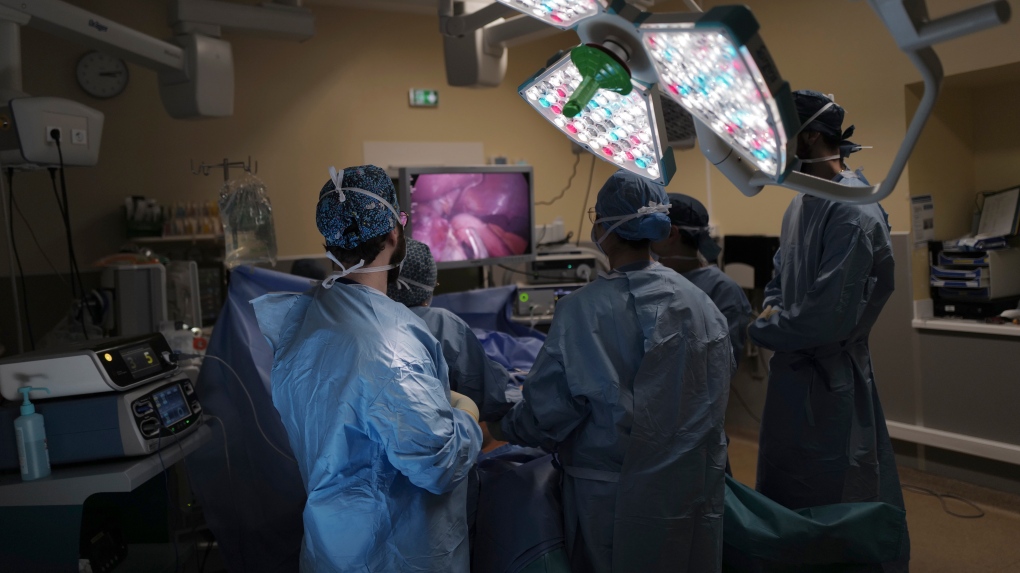
Imagine having a potentially shorter wait time for surgery or having ready access to a second - or possibly third - opinion on your diagnosis. In many pockets of Canada’s vast and complex health-care system, physicians have worked effectively for years as a team under a “shared-care” model. Some surgeons are hoping this form of patient care can be widely adopted across surgical specialties, especially in the wake of the COVID-19 pandemic.
The strain placed on the system over the last two-and-a-half years prompted the head of the Canadian Medical Association, Dr. Katharine Smart, to warn in June that “the collapse of the current health-care system” is coming. Overworked nurses and doctors, staffing shortages, emergency rooms closures, and a backlog of surgeries during the worst periods of the pandemic are just a few of the many challenges that have exposed long-standing systemic issues, proving just how fragile Canada’s health-care system is. Meanwhile, concerns around patient care and surgical wait times – already an issue prior to the COVID-19 – have been exacerbated by the pandemic.
“Every time we've had a surge, there's been a shutdown. There's been a lot less predictability around resources, and particularly surgical resources,” Dr. Fady Balaa, an associate professor of surgery with the University of Ottawa, told CTVNews.ca in an interview this week.
“These kinds of models make you a lot more nimble, that you can tolerate this unpredictability a lot better and respond to this unpredictability a lot better.”
There are variations to the team-based or shared-care model and different levels of integration. In surgery, it broadly means that patients do not deal exclusively with one surgeon, but are under the care of a team of surgeons. Any one of them may ultimately perform the surgery.
The traditional model in Canada saw most surgeons in some form of solo practice, explained Dr. Sean Cleary, president of the Canadian Association of General Surgeons.
“Everybody was an island,” Cleary told CTVNews.ca in a phone interview on Thursday.
“One surgeon in town might have an eight-month waitlist for a problem whereas another surgeon might have a waitlist of two months to see a certain patient and so it created these inequities and disparities in care….it also perpetuated some of the stereotypes and biases that we had in society.”
Cleary said these included gender and referral biases, the notion that surgeons practiced independently, and that the busier they were, the better surgeon they were.
“Which was not always the case,” he said.
SUCCESSFUL EXAMPLES
To be clear, the shared-care model is not new to surgery – obstetrical care, bariatric and emergency department surgeries, for example, have been operating in a team environment for years, and from Cleary’s perspective, more and more surgeons are moving towards this model, not only in academic environments, but also in smaller communities where managing the long hours of a solo practice is unsustainable.
Dr. Nancy Baxter, currently the head of the Melbourne School of Population and Global Health at the University of Melbourne, says it was not very common in acute care surgery when she first began practicing, but is now routine. And she has seen a clear move towards this model for certain types of procedures like liver surgery, where patients can be quite sick afterwards and a great deal of post-operative care is required.
“Team-based care benefits patients in that there tends to be greater surgeon availability,” she explained via email on Thursday. Baxter, who spent 15 years in Toronto, was previously a general surgeon with the Department of Surgery at the University of Toronto until 2020.
“If a surgeon is caring for ward patients for the week they will spend more time on the ward then they would if they were caring for only the few patients they had operated on. The nurses and allied health professionals know who is covering the ward so it is easy to identify who should be called if there is a problem.”
Balaa, who was the former division head of general surgery at the University of Ottawa and practiced under a team model for more than 17 years, is seeing more new graduates setting up their practices this way as well.
Dr. Susan Moffatt-Bruce, the chief executive of the Royal College of Physicians and Surgeons of Canada told CTVNews.ca that team-based care, particularly in surgery, is “foundational” in providing high quality care.
“We have an opportunity in Canada to embrace team-based models with the patient at the center of care,” she said in an emailed statement on Thursday.
“This enables all health care professionals, including specialist physicians, to work to their highest potential and ability. Fortunately, we are seeing team-based care evolve. Ultimately it will provide the highest level of efficiency and quality.”
Still, surgeons say this model remains less common for most types of elective surgeries.
An elective surgery does not necessarily mean the procedure is “optional.” The term refers to any surgery that can be scheduled in advance and is not required due to an immediate, life-altering or life-threatening emergency.
“What we're after is more wider adoption…the public's been OK with this being a model for any kind of emergency surgery,” Balaa said, noting that some of the resistance has stemmed from concerns over its feasibility in very complex surgical cases.
“I think, if built right, there's no reason why this can't be done in an elective setting and in cancer populations.”
Wait times are an enormous source of pressure, he says, and harmonizing this practice model across surgical disciplines would reduce the imbalance and bottleneck of having some surgeons with long wait lists and others with short ones. He believes physicians, patients, and the health-care system would benefit from an overhaul away from traditional referrals and solo practices.
Baxter, however, is more cautious and says she is unsure how much it would help wait times.
"The key thing for surgical wait times is OR availability, ensuring optimal use of surgeon resources through case distribution, and avoiding low-value surgery."
Low-value surgery are typically procedures that are costly and have limited upside for patients, or where the risks outweigh the benefits.
PATIENT OUTCOMES AND SAFETY
Earlier in September, Balaa and his colleagues presented research at the Canadian Surgery Forum that demonstrated the feasibility and safety of a shared-care model of practice – even with highly complex elective surgeries, like those for pancreatic cancer. They say the model could improve patient care, provide more support for surgeons, and help make the system more efficient.
They reviewed the outcomes of 174 patients who underwent a pancreaticoduodenectomy in a shared care practice between January 2016 and December 2020. The median number of surgeons involved in a patient’s care was three.
Also known as a Whipple procedure, this surgery is considered a major operation for removing cancerous tumours in the pancreas. The Mayo Clinic describes it as “a difficult and demanding operation” that can have serious risks, but can also be a lifesaving procedure, particularly for cancer patients.
For this review, they analyzed patient outcomes for several metrics including 30-day mortality, sepsis, unplanned return to the operating room, surgical site infections, and readmission. They found that a shared-care model was feasible even for complex surgeries “without compromising patient outcomes and safety.”
HOW PATIENTS AND SURGEONS BENEFIT
Even before they see a surgeon, patients can face long wait times just for referrals. On this front, there is growing advocacy among doctors for some type of single-entry, or single-queue model – where patients go through a centralized system and are seen by the first available specialist instead of waiting for a specific one. Proponents say it is an equalizer that is also more efficient, because there are multiple providers behind the single queue. The shared-care model is the next phase beyond the entry into the surgical system, Balaa explained.
Though far from universal, “we're seeing wider and wider adoption of single-entry models,” he said.
But the invisible queues do not end there, doctors say. Once a patient is assigned to a specific surgeon, they may need to navigate multiple additional queues, including a surgeon’s availability and when that surgeon has access to the operating room.
Broad adoption of some type of shared-care model would not only help alleviate the many barriers that patients encounter throughout their surgical care journey, but also help encourage more support and collaboration among surgeons as well, Balaa says.
Surgeon interchangeability and having simultaneous involvement in patient care is helpful at all stages of their careers, but especially when dealing with challenging cases, he explained. At the same time, early career surgeons can also benefit from the experience of veterans. Those in the later stages of their career may also find the collaborative environment a helpful means of transitioning out. It is also a more “supportive and collegial environment” to practice in, supporters say, particularly valuable given the burnout many physicians have been experiencing over the last two-and-a-half years.
“Without team-based care, a surgeon would have a full schedule every day and spend only a small amount of time on the ward,” Baxter said, adding that if a surgeon’s patient became ill, caring for them would mean delays or cancellations to other booked appointments and surgeries. Scheduling is also easier in other ways. There is less pressure to find coverage for patients, because the rest of the surgical team is ready to step in.
Cleary also believes that these kinds of shared models are helping their specialty achieve better equity and gender balance. But Baxter noted that in practice, this does not shield surgeons from facing discrimination on the job, pointing to examples where patients complain over not having been seen by a doctor, despite being visited by a female physician on a daily basis.
For patients, it can mean benefiting from more than one expert opinion regarding their medical care, and more attention from the surgeons themselves.
“You start to build a bit more redundancy into the model where maybe it's a bit safer because more than one surgeon has had her or his eyes on the case and opinion about the case,” Balaa said.
Cleary agrees. “They’re getting more efficient care, and when we make decisions as a group, we make better decisions.”
DRAWBACKS AND CHALLENGES
This type of model is not without its downsides, however.
From a patient’s perspective, some of the personal, individualized contact is lost. The surgeon caring for them may be different from the one who ultimately does the operation. In the analysis by Balaa and his colleagues, 100 patients, or just over 57 per cent, met their primary operating surgeon for the first time at the time of the surgery.
“The downside for patients is that they will be cared for by someone they may never have met before surgery and that can be challenging,” said Baxter.
“Also, if they have a problem that results in them being in the hospital for some time, they will have a different physician caring for them every week.”
It is an issue Balaa acknowledges.
“There's something really special about the relationship between a surgeon and her or his patient. Trust sits at the core of that.”
For surgeons, challenges include an increase in the number of handovers and making sure that the exchange of information is seamless and complete. If there are no standard protocols in place, different surgeons may have different approaches to patient care.
This type of model requires a great deal of trust in the other surgeons, Baxter said.
“You may take over a patient who was not cared for in a manner consistent with your judgment – that can be challenging and you can end up with liability for the patient’s outcome.”
For these, and other reasons, some surgeons remain resistant to the idea, experts say.
In some practices, this model can also mean a reduced income for surgeons, Baxter noted, which may also be another source of resistance.
More broadly, another challenge Cleary noted is that in provinces like Ontario, the health-care system is not set up to support surgeons in a shared-care model and it has yet to evolve in that direction.
Meanwhile, Balaa says his research should at least alleviate concerns around the feasibility and safety of complex surgeries under this model.
“I'm in no way pretending that this is going to be a fix for all the problems or even a definitive fix for any single problem,” he said, but if surgeons began considering their practices from a team-based perspective, it would help mitigate some of those pressures.
“It's not going to solve the nursing shortage, it's not going to solve the equipment shortages, and it's not gonna stop the budget shortages. But as we see resource constraints becoming more and more real, we have to look at the most efficient ways we can use these resources. And we have to continue to focus on building really supportive environments, because we see the toll this has taken on health care providers.”