TORONTO -- One of the main tools used in hospitals during the pandemic has been the ventilator, a machine that supports the breathing of those battling a severe case of COVID-19 — but after weeks or months on a ventilator, recovering patients can struggle to swallow, eat, drink or even to speak.
That’s where speech-language pathologists come in, fulfilling an essential, but little-known role in the frontline response to this pandemic.
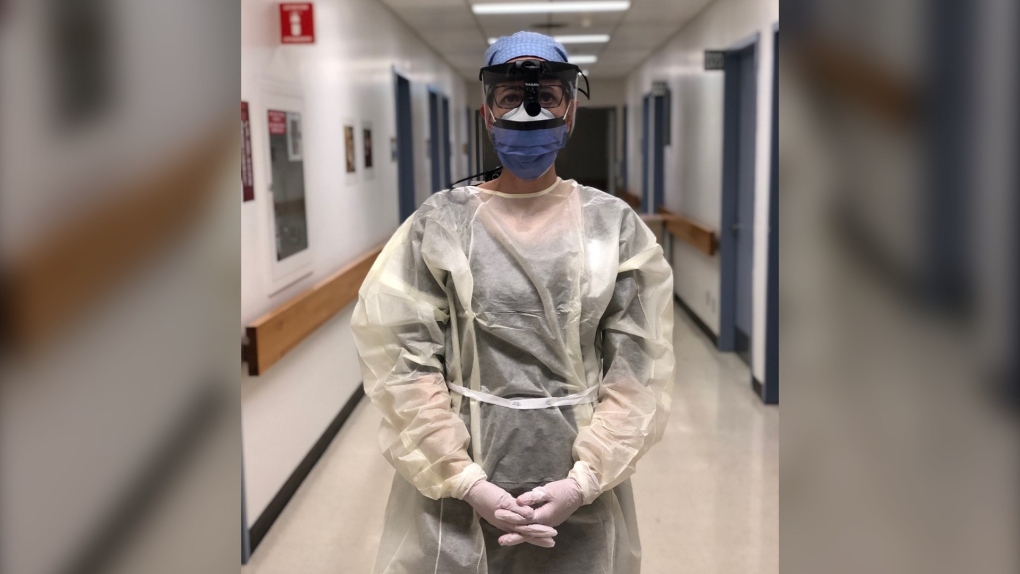
Avital Winer is a speech-language pathologist who works with The Ottawa Hospital, and has firsthand experience supporting COVID-19 patients in their recovery process, walking them through simple processes like drinking water again without a tube in their throat.
“Eating and drinking is so fundamental to who we are as social creatures,” she told CTVNews.ca by email. “It can be hard to imagine what it's like not be able to swallow a sip of water, let alone eat your favourite foods.”
Speech-language pathologists (SLPs) working in acute care assess and manage any issues a patient may have with communicating, whether it be a physical issue or a cognitive one. But a big part of their job is also assessing and managing issues with swallowing that may have arisen from medical conditions or treatment.
Swallowing disorders are called dysphagia, and can affect numerous aspects of a person’s ability to communicate or function normally.
And being treated for a serious case of COVID-19 can inadvertently lead to dysphagia.
“With respect to COVID-19, dysphagia management does constitute a considerable portion of the intervention required for these patients,” Winer said.
Around 40 to 60 per cent of COVID-19 patients who have to be on a ventilator for a prolonged period during their illness experience post-extubation dysphagia in the aftermath, Winer told CTVNews.ca in an email.
“Dysphagia in some can occur after 48 [hours] intubated, but likelihood increases significantly following intubation of 5-10 days,” she said.
Although detailed hospitalization information isn’t available for every case of COVID-19 in Canada, the most recent epidemiological summary put out by the Government of Canada stated that at least 1,500 people have required mechanical ventilation.
COVID-19, SPEECH AND DYSPHAGIA
Winer explained that there are several mechanisms that contribute to dysphagia and struggling with speech in these COVID-19 patients.
One factor is that having a tube inserted into your throat may cause trauma to the larynx itself. The longer that a person is intubated, the more likely it is that they’ll struggle to speak at first.
“The vocal cords, through which the breathing tube passes, is the gatekeeper to the airway. If they do not work properly- if one or both vocal cords are weak, paralyzed, significantly swollen for example- this can result in inefficient airway protection, and result in aspiration,” Winer said.
“Prolonged or repeated intubations can result in increased trauma to the vocal cords. And, if there is vocal cord trauma […] this will also impact an individual's ability to use their voice, and communicate.”
COVID-19 patients may have muscular weakness related to being critically ill, which affects their swallowing.
They may also have suffered cognitive complications from COVID-19 or their time spent unconscious, which makes for yet another hurdle as they relearn to swallow and communicate.
Sarah Jane Garland, director of adult services with Speech and Hearing BC, told CTVNews.ca by email that while SLPs have standard methods of helping other patients with issues with swallowing, it’s very different working with COVID-19 patients.
“The recovery process for someone with a stroke is well known and predictable but the recovery process for someone with COVID-19 is not as predictable,” she said.
She added that patients who are experiencing cognitive struggles will have a harder time following instructions given to them by SLPs which are meant to help them.
It’s not surprising that COVID-19 patients would experience dysphagia after being intubated, according to Dr. Stacey Skoretz, a speech-language pathologist and assistant professor at the University of British Columbia (UBC).
“Following critical illness, my research has shown that if someone needs to be on a breathing machine for longer than 48 hours, approximately 2 out of every 3 people will have a swallowing problem afterward,” she told CTVNews.ca in an email.
“Emerging evidence suggests that the frequency of swallowing disorders in those with severe SARS-CoV-2 infection that also need to be on a breathing machine may be higher.”
One of the big dangers of not being able to swallow correctly is the risk of aspiration, which is when food or liquids go the wrong way into the lungs. While a person swallows, Winer explained, the body naturally holds the vocal cords closed so that food or liquids don’t enter the airway. But for seriously ill COVID-19 patients, balancing breathing and swallowing isn’t always automatic anymore.
“This pattern can be seen in patients following extubation, and we are also seeing this in our COVID-19 patients who have not been intubated, but are very short of breath nonetheless,” Winer said.
Inhaling food or liquids into the lungs can cause aspiration pneumonia, “which can be dire for someone who is already critically ill,” she said, and can extend their hospital stay.
People suffering from COVID-19 are only put on a ventilator as a life-saving measure when their oxygen levels drop dangerously low, and they cannot take in enough air on their own. But it comes with these complications for recovery.
“We often take eating, drinking and communicating for granted,” Skoretz said. “During severe illnesses, including those requiring life saving measures such as mechanical ventilation, survival is the priority.”
LEARNING TO SWALLOW AGAIN
After a patient has been extubated, if there appear to be any issues with swallowing, eating, drinking and/or communicating in general, that’s when an SLP is called.
They can help patients communicate with the team caring for them, as well as their family, while working on their assessment of the patient.
“We try to determine if the patient can safely swallow with low risk of aspiration, what they can swallow safely, and how to help them swallow safely with appropriate strategies, postural maneuvers, or changes in texture,” Winer said.
In any other situation, SLPs might observe the inside of the patient’s throat using an endoscope to find where the breakdown in swallowing is occurring. But it’s not so simple now.
“One of the challenges we have encountered during this pandemic is that these tests cannot be used for these patients if they still have an active COVID-19 infection,” Winer said, explaining that more risks are associated with moving the patient out of isolation to perform the test, and that the test risks “aerosolization of the virus.”
“So we have had to get around that and really rely on our clinical skills.”
SLPs may work with otolaryngologists — also known as ear, nose and throat doctors (ENT) — if a speech issue is related to “persistent vocal cord paralysis,” but speech therapy itself depends on the patient’s recovery progress.
It can be a long process for patients to recover their faculties completely. Some patients who are assessed in acute care will go on to be referred to a clinic focused on rehabilitation, where they will receive ongoing speech therapy, or will receive that therapy as an outpatient. In the hospital where Winer works, there is a rehab clinic onsite that patients can attend.
Winer said she believes the work load for SLPs in Canada has gone up as a result of the pandemic, but although a few studies have looked into dysphagia during the pandemic, there still isn’t a lot of data on it yet.
One U.K. study that came out last November looked at around 730 COVID-19 patients, and identified that out of the 208 patients who were referred for swallow assessment, 102 of them had been admitted to the ICU for mechanical ventilation support.
A study performed in Belgium that was published last month and only looked at 21 patients who had been on ventilators found that 90 per cent of them “presented impairment in their swallowing function.”
Skoretz is currently carrying out research in this field at UBC, focusing on “understanding the multiple systems involved in swallowing following the use of breathing tubes and ventilators after critical illness, including those with COVID-19.”
She is aiming to shed more light on how best to rehabilitate patients, and said her team will be sharing their findings in the coming months.
“Relative to other illnesses, we are in the early days of understanding the effect of COVID-19 on the upper aerodigestive tract,” she said.
Relearning to speak or struggling with swallowing is part of the recovery process from COVID-19 that isn’t often talked about, but it affects many patients, according to SLPs.
“I think it’s surprising we don't hear more about post-extubation dysphagia given the prevalence,” Winer said.
"I think most people think SLPs [only] treat kids with speech and language disorders so this isn't an area of practice that has great visibility.”
She said that most people aren’t aware of this type of medical care — both swallowing and communication disorders in adults — until they or someone in their life needs this care.
But although their work during this pandemic has gone unseen by the general public, it’s still something Winer and other SLPs are proud of.
“Being able to help patients take their first sips of water, after potentially weeks of nothing to eat or drink by mouth, usually makes you a pretty welcome part of the care team,” Winer said.
“And [it is] pretty special to be able to contribute to an individual's care in that way.”
----
Have you gone through speech therapy during the pandemic? Email us at dotcom@bellmedia.ca with your name, location and contact information, as well as some details about your situation, and we may get in touch.