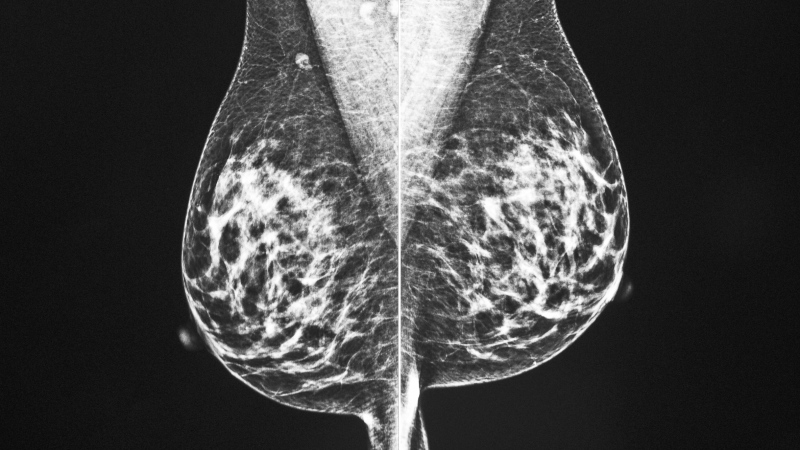
HALIFAX -- A Nova Scotia woman has reached a settlement with the province in a human rights complaint that was launched after she was denied breast reduction surgery.
Halifax resident Melody Harding made a complaint against the province and the Department of Health in August 2017 after she was told she wouldn't receive coverage under the province's health insurance plan for the procedure because her body mass index was above the threshold required.
Harding maintained the policy was discriminatory.
According to a three-page settlement decision by an independent board of inquiry, the province has agreed to remove a requirement that a person have a body mass index of 27 or less to be considered for breast reduction surgery. It will instead assess the medical need for the procedure on a case-by-case basis.
Body mass index is calculated using a person's weight and height. According to federal guidelines, someone with a score of 25 or higher is considered overweight and 30 or higher is considered obese.
The Health Department is now required to advise Nova Scotia physicians about the change in policy.
Although both sides have agreed to keep the terms of the settlement agreement confidential, the inquiry board describes the outcome as "being in the public interest in the circumstances of this case."
Harding said in a news release issued Monday that she is "so pleased to have found common ground" with the Health Department.
"Removing the body mass index restriction from the breast reduction surgery criteria is such a positive development for the women in Nova Scotia that are effected by macromastia, myself included," she said.
The inquiry board's decision said that under the terms of the agreement, the province will provide coverage when 400 grams or more of tissue need to be removed from each breast and there are documented physical symptoms attributed to the size of the breasts including neck or back pain or other symptoms.
"The parties are to be commended for their efforts in resolving this matter," wrote Gail Gatchalian, the board of inquiry chair.