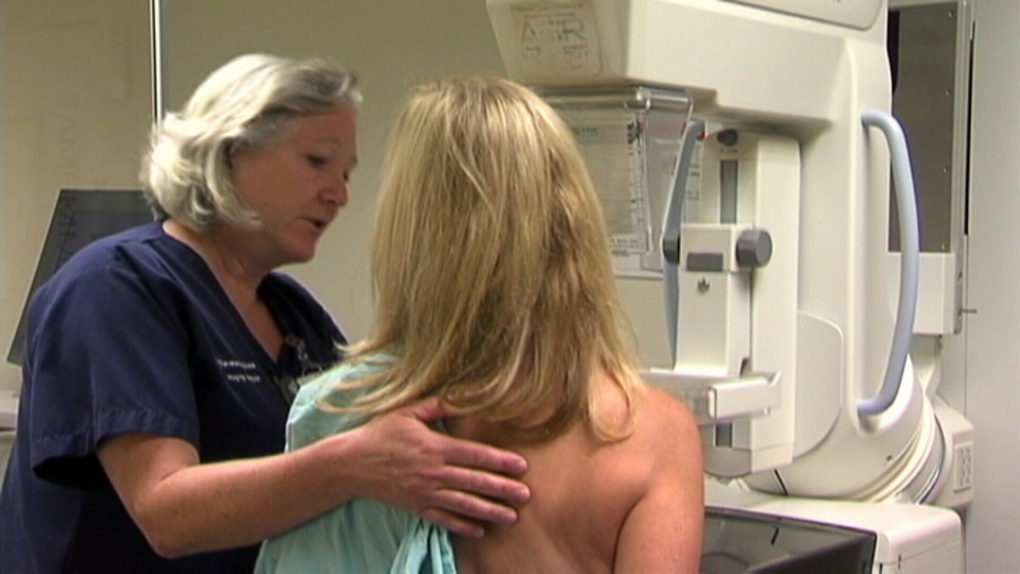
While recently published studies on the effectiveness of mammograms may lead to confusion among patients, individual consultations with a physician can help them make informed choices about their screening options.
According to CTV medical expert Dr. Marla Shapiro, anyone who is unsure about the necessity of regular mammograms needs to chat with their family doctors so a decision can be made that is in the best interest of the patient. “We don’t women walking away feeling that there’s no point in doing this,” she said.
A study published last week in The New England Journal of Medicine found that mammograms are having only a small impact on breast cancer-detection rates and have led to more than one million women being overdiagnosed with the disease in the past 30 years.
The study found that between 1976 and 2008, nearly in 1.3 million U.S. women were overdiagnosed, meaning the tumours detected by the mammograms would never have progressed into the full-blown disease.
In addition to the NEJM study, two other studies on the issue were recently published.
In the first, an independent U.K. panel presented its review of the benefits and harms of breast cancer screening in the medical journal The Lancet. The panel found that screening reduces breast cancer mortality, but some overdiagnosis does occur. Specifically, the panel found that for every breast cancer death prevented, three cases were overdiagnosed.
The researchers found that for every 10,000 women in the U.K., aged 50, who are screened for the next 20 years, 43 deaths from breast cancer would be prevented and 129 cases would be overdiagnosed.
The study also found that many women felt that getting a mammogram is worthwhile.
In a second study released Tuesday, researchers analyzed data from New York Presbyterian Hospital Weill Cornell Medical College on screening mammography between 2007 and 2010. They found that out of 43,351 screening exams, 205 breast cancers were detected.
Of those that were detected, nearly 20 per cent were found in women in their 40s and half of those were invasive. The authors of the study noted that it would be unacceptable to potentially miss those cases.
“Their concern is that if we’re not doing any screening for those women between the ages of 40 and 49, we’re missing these cancers,” said Shapiro.
While the results of these studies can be confusing, Shapiro said patients can make an informed decision about their personal screening options by talking to their doctors about the risks and benefits of screening.
Shapiro recommends that patients sit down with doctors and discuss their options and other risk factors such as family history, breast density, physical activity levels, alcohol consumption and weight.
Shapiro said she often has this discussion with her own patients.
“When I have a conversation with women in my office everyday explaining to them that we may overdiagnose you, meaning we’ll find something that may never get you into trouble. Many (more) of them feel that they can tolerate that level than not,” she said. “There are some who say ‘No, I’m going to wait till I’m 50, I’m not interested.’
“We’ve got to have that one-one-one issue. I understand the ‘Let’s not screen everybody,’ but let’s not throw the proverbial baby out with the bath water.”