With several measles outbreaks currently underway in Canada, many Canadians are wondering if they might be at risk for the potentially fatal illness.
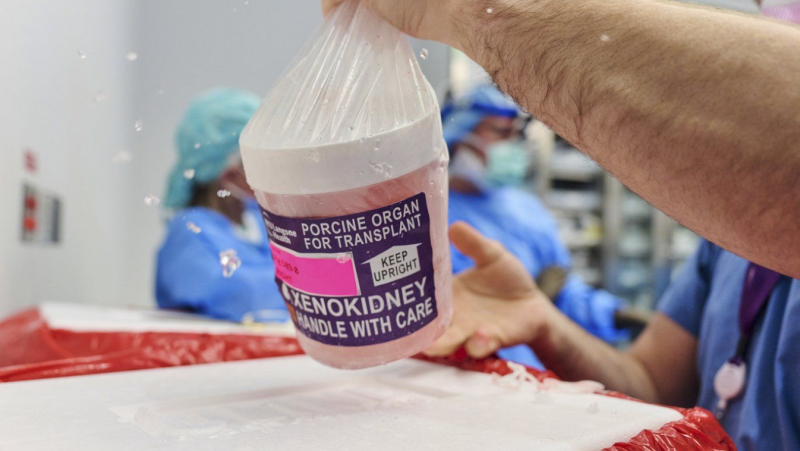
In British Columbia's Fraser Valley, there is currently a large outbreak involving more than 225 patients that began in an unimmunized religious group. Two more clusters are underway in central Alberta and Manitoba and a handful of cases in southern Ontario and Ottawa. Several of these cases occurred in people who have recently travellers to the Philippines, which is in the midst of a major measles outbreak involving more than 15,000 suspected cases.
Here are some tips to determine if you are at risk.
How do I know if I've been vaccinated?
All children born after 1963 should be vaccinated against measles. The vaccine is combined with the vaccines for mumps, rubella and sometimes varicella (chickenpox), so it will appear on your vaccination card as either MMR or MMRV.
The first shot is typically given to babies around their first birthday. A booster shot is then given around 18 months, or between four and six years old, depending where you live.
Sometimes the shots are given before a child is 1 year of age if the child is travelling to an area where measles is common or if there is a measles outbreak near them. The Canadian Paediatric Society says it's even safe to give the second shot as soon as one month after the first one.
In 1996 to 1997, every Canadian province and territory added a second dose of measles-containing vaccine to its routine immunization schedule, and most conducted catch-up programs in school-aged children.
If you don't know whether you were vaccinated as a child, you could try contacting your parents or the family doctor you had as a child, who might still have a record. Public health units also keep records.
Dr. Allison McGeer, the head of infection control at Toronto's Mount Sinai Hospital, says if that doesn't work, it's best to talk to your doctor or health provider to find out which vaccines are most important for you to have. Then, he or she can order blood tests to determine your immunity.
How effective is the vaccine?
If you received both doses, there is a very good chance you are completely protected, since the efficacy of a single dose given at 12 of age is estimated to be 85 to 95 per cent, while the efficacy of the second dose is almost 100 per cent.
For those who suspect they only ever had one dose of the vaccine, it's worth discussing with your health provider whether you should a booster shot. Those considered at greatest risk of exposure include travellers to destinations outside of North America, health care workers, students in post-secondary educational settings, and military personnel.
If there is an outbreak of measles in your area and you are not sure if have received two doses, it is best to speak to your doctor or health provider.
What if I was born before the measles vaccine became available in 1963?
The Canadian Public Health Agency of Canada says that adults born before 1970 can be presumed to have acquired natural immunity to measles, because the disease was circulating widely in those years. However, health care workers, military personnel and travellers to destinations outside of Canada should receive the MMR vaccine, regardless of year of birth to ensure they are protected.
What if measles mutated since I was vaccinated?
The measles virus is not like influenza and does not mutate significantly from year to year. Dr. McGeer says there’s no evidence that measles is changing in any way.
If I'm not vaccinated, how likely am I to get sick?
Measles is considered more contagious than almost any other disease.
You can catch measles just by being in a room where a person with measles has been -- even after that person has left a room. That's because the virus can hang in tiny water droplets in the air for hours. And almost everyone who has not had the vaccine will get measles if they are exposed to the virus.
Even if you do not become very ill, you can spread the illness to children who might become severely ill. And it is possible to spread measles even before you develop a measles rash.
Is measles really that dangerous?
Measles is no picnic. It causes a very high fever, breathing problems, and a nasty rash that spreads over the entire body. Most people eventually recover, but in children, about one in 10 will also get an ear infection, and up to one in 20 will get pneumonia. The CDC says that in 2011, 38 per cent of children younger than 5 who had measles had to be treated in the hospital.
In severe cases, measles can cause encephalitis, which is a swelling of the brain that can lead to permanent brain damage. Other children will become deaf from the encephalitis.
And of course, there is the risk of death. Before vaccines were available, measles killed several hundred Canadians each year. And there is no way to cure measles; doctors can only treat its symptoms.
In pregnant women, measles can cause a miscarriage or premature birth. The older a person is, the worse the risk of complications from these illnesses, which is why the MMR vaccine is given at a young age.
Why don't we have a central registry to keep track of our vaccines?
Dr. McGeer says it would be great if Canada had a national online registry where Canadians could look up which vaccines they've received and which ones they might still need. But she says that it's unlikely our country will ever have one.
The difficulty is two-fold, she says. First, Canada doesn't have a national health system, we have provincial systems so it's difficult to create a registry that would be accessible all across the country. Secondly, it would be difficult to set up a system in which any health practitioner could access the info they need to, while preserving a patient’s privacy.
McGeer says as alternatives, there are already some good apps and websites available where patients can record their immunization history.
Who should not get vaccinated?
Anyone who has ever had a life-threatening allergic reaction to the antibiotic neomycin should not get the vaccine. Nor should anyone who had a life-threatening allergic reaction to a previous dose of MMR vaccine.
Pregnant women should not get MMR vaccine because pregnancy changes their immune system. They should wait until after giving birth.
The following patients may be able to get the vaccine but should speak to their doctor:
- those with HIV, or another disease that affects the immune system
- those taking drugs that affect the immune system, such as steroids
- those being treated for any kind of cancer
- those with blood disorders or those who have ever had a low platelet count
- those who recently had a blood transfusion or received other blood products