TORONTO -- A Canadian health expert believes a lack of resources on an international level led to the limitation of how many Canadians could be tested for COVID-19, but says other testing options are on the horizon.
As the virus spread through Canada, provincial health authorities began limiting those who required testing to those with serious symptoms, pre-existing conditions, health-care workers or those who had travelled outside the country. Meanwhile, those with mild symptoms, such as cough, sore throat and runny nose, were told not to get tested and instead self-isolate.
Dawn Bowdish, Canada Research Chair in aging and immunity at McMaster University, told CTVNews.ca that only testing the more serious cases has led to a wider community spread within Canada, but that authorities are doing the best they can with the limited resources they have.
“I think they've done a great job in scaling up the capacity and these people are working extremely hard to do these tests, but even if you have the people power and the capacity, if you can't get the supplies, then you could still be limited,” she said in a recent phone interview.
Because the virus spread in several countries before arriving in Canada, local authorities were able to plan ahead, but were left with few supplies due to the global demand.
“The disadvantage to coming late to the game was that the entire world uses the same resources, the same swabs for testing people's nose, the same reagents for doing the test and, unfortunately, that means that there's been a huge demand on these resources and we simply don't have enough resources,” she said in a recent telephone interview.
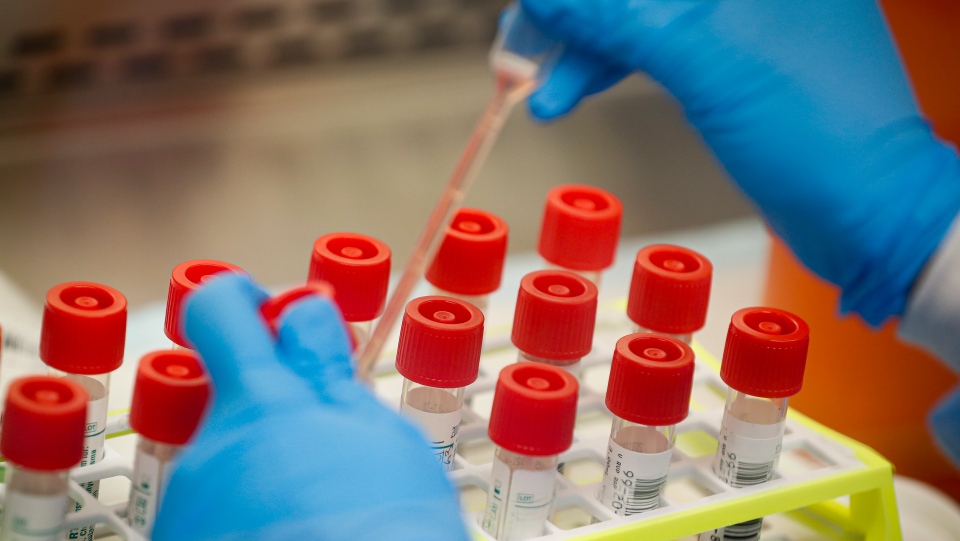
Bowdish added that one of the few tests scientists are confident with involves a special kind of nasal swab that, prior to the outbreak, was mostly made in Italy, among the hardest-hit countries in the world.
“(Nasal swabs are) trying to be sourced from China and other places, but it takes time to validate those,” she said. “So right now, we literally do not have enough swabs to do all the testing that we know we need.”
In Ontario, provincial health authorities have not tested more than 5,000 people in a day since April 2, despite a capacity to test more than 13,000.
“We are going forward on a rapid fashion to make sure every single person possible can get tested,” Ontario Premier Doug Ford told reporters on Wednesday. “After our front-line health-care workers and first-responders, we need to be testing everyone.”
To help ramp up testing, the province is changing its guidelines to include atypical symptoms such as: unexplained fatigue, chills, nausea and delirium.
Zain Chagla, director of infection control at St. Joseph’s Healthcare Hamilton in Hamilton, Ont., told CTV News that these changes will cut down on people who might be spreading COVID-19 while they believe they might have some other illness.
“I think all of us have been a bit surprised in people that we think are relatively low probability in our minds and have some mild symptoms like diarrhea and muscle pain and show up positive and obviously we don't want to be missing those cases,” he said.
Meanwhile, British Columbia, Alberta, Manitoba and Quebec have all previously reported a backlog in testing.
Solutions appear to be on the way, however. Last week, Prime Minister Justin Trudeau announced the government had purchased more than a million test kits, while Bowdish adds several Canadian entities are looking at new ways to ease the backlog of testing.
“I have a strong suspicion that we're going to see a big upswing in testing in the next few days, but this has required people to be incredibly resourceful in trying to find new ways of doing the same tests that give us the same quality results,” she said.
BLOOD TESTING COULD BE ON THE HORIZON
One of these unique solutions could be blood testing, Bowdish said. While not all that effective while someone is sick, a serological test measures the amount of antibodies present in the blood stream, which could tell if someone had contracted the virus previously and developed an immunity.
“This will allow us to understand how many people are asymptomatic versus symptomatic, how far it spread, which communities are the most affected and will be very important for planning the next outbreak,” Bowdish said.
One of the benefits of serological testing, Bowdish said, is that understanding who has the antibodies can allow you to rearrange a workforce for optimized safety.
“The phrase we use is called ‘redeployments,’ and that's when you shift people around based on their risk,” she said. “You can imagine that our nursing homes, where we've had a huge issue with health-care workers becoming infected and working with vulnerable patients, you could see how valuable it would be to know who was not going to be spreading the disease.”
Similarly to the nasal swabs, however, these tests are also in high-demand, however.
Other testing options are in the works as well. Last month, Alberta and Ontario announced they signed deals with Spartan Bioscience Inc., to provide handheld testing devices that promise results in less than an hour, though it’s not clear when the devices will be available for use.
With files from CTV News Corresdondent Heather Wright