After studying the correlation between the sleep disorder narcolepsy and H1N1, scientists have discovered that the body’s immune response to the virus may trigger narcolepsy in genetically predisposed patients.
The virus, which is the predominant flu strain in North America today, spread around the world in 2009, and was declared a pandemic by the World Health Organization.
But researchers now say the outbreak did more than cause a nasty swine flu. It triggered cases of narcolepsy around the world -- a disease characterized by sudden, uncontrollable sleepiness and muscle weakness, caused by the body’s immune system mistakenly destroying brain cells that make hypocretin -- a “wakefulness” protein.
A sudden increase in the number of narcolepsy cases was observed in a 2010 study in China, which showed a rise in sudden onset narcolepsy in children living in areas where the H1N1 pandemic had spread the previous year.
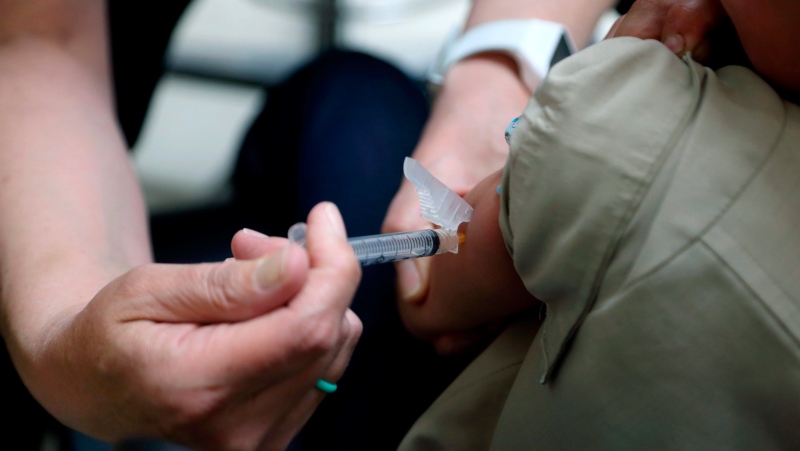
At the same time, clinicians in Scandinavia noticed cases of narcolepsy in children who had been vaccinated with Pandemrix, a newly developed anti-H1N1 vaccine, which was meant to induce a stronger immune response to the virus, and which may have triggered narcolepsy in a few thousand patients in Europe.
In a new study published Wednesday in Science Translational Medicine, researchers found that immune cells that tried to destroy the H1N1 virus also attacked and destroyed similar looking cells in the brain (hypocretin), in patients genetically predisposed to narcolepsy.
The immune system attacked both cells through a phenomenon called “molecular mimicry,” leaving patients with narcolepsy.
Dr. Emanuel Mignot at the Stanford School of Medicine told CTV News that researchers are now “proving without a shadow of a doubt that narcolepsy is an autoimmune disease because we have found the exact target that the immune system is attacking.”
Meanwhile, Dr. Brian Murray at the Sunnybrook Health Sciences Centre, said the study is very important to understanding the biology of the condition, which will help doctors develop better treatment for the disease.
“Early diagnosis could be quite beneficial to the patient because they can get on therapy in a more timely fashion,” he told CTV News.
The study suggests ways of intervening before the complete destruction of hypocretin brain cells, and could pave the way to a new blood test to diagnose the disease, which at the moment can take over a decade to get properly diagnosed.
Scientists are also now beginning to question whether other brain disorders, such as schizophrenia, are linked to autoimmunity.
“People have long thought that the brain is somewhat immune to autoimmune diseases,” Mignot said in a press release. “But we’re learning this is wrong.”
With a report from CTV's medical specialist Avis Favaro and producer Elizabeth St. Philip